Understanding the Complex Connection Between Mental Health and Addiction
Mental health addiction refers to the co-occurrence of a mental health disorder (like depression or anxiety) and a substance use disorder. These conditions often appear together and influence each other, creating a cycle that can be difficult to break without proper treatment.
Key Facts About Co-Occurring Disorders:
- 19.4 million adults in the U.S. with substance use disorder also have a mental illness
- 6.4 million adults with serious mental illness also have a substance use disorder
- Either condition can develop first, or they may emerge simultaneously
- Treating both conditions together (integrated treatment) leads to the best outcomes
- Recovery is possible with proper diagnosis and evidence-based care
Historically, addiction was seen as a moral failing. Today, research confirms mental health addiction is a treatable brain disease requiring comprehensive, integrated care. Both conditions alter brain chemistry, share risk factors like trauma and genetics, and often lead to self-medication to cope with symptoms.
The relationship is bidirectional: a person with depression might use alcohol for relief, worsening their depression, while someone using cocaine might develop anxiety. In other cases, both conditions stem from shared risks like childhood trauma or genetics.
At Drug Rehab Headquarters, we help individuals and families steer mental health addiction and recovery. We connect people with specialized centers offering the integrated care needed for lasting recovery from co-occurring disorders.

Key mental health addiction vocabulary:
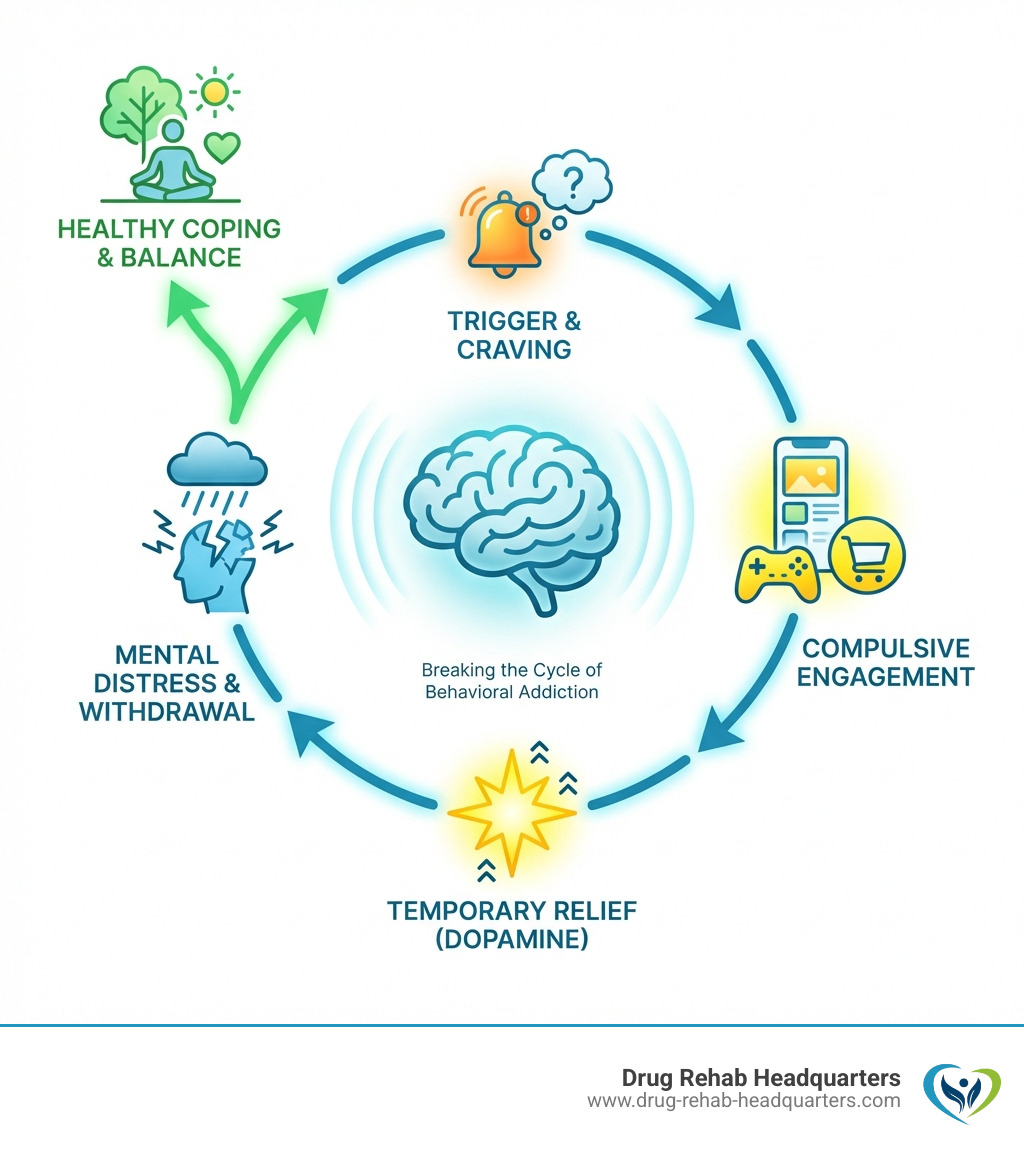
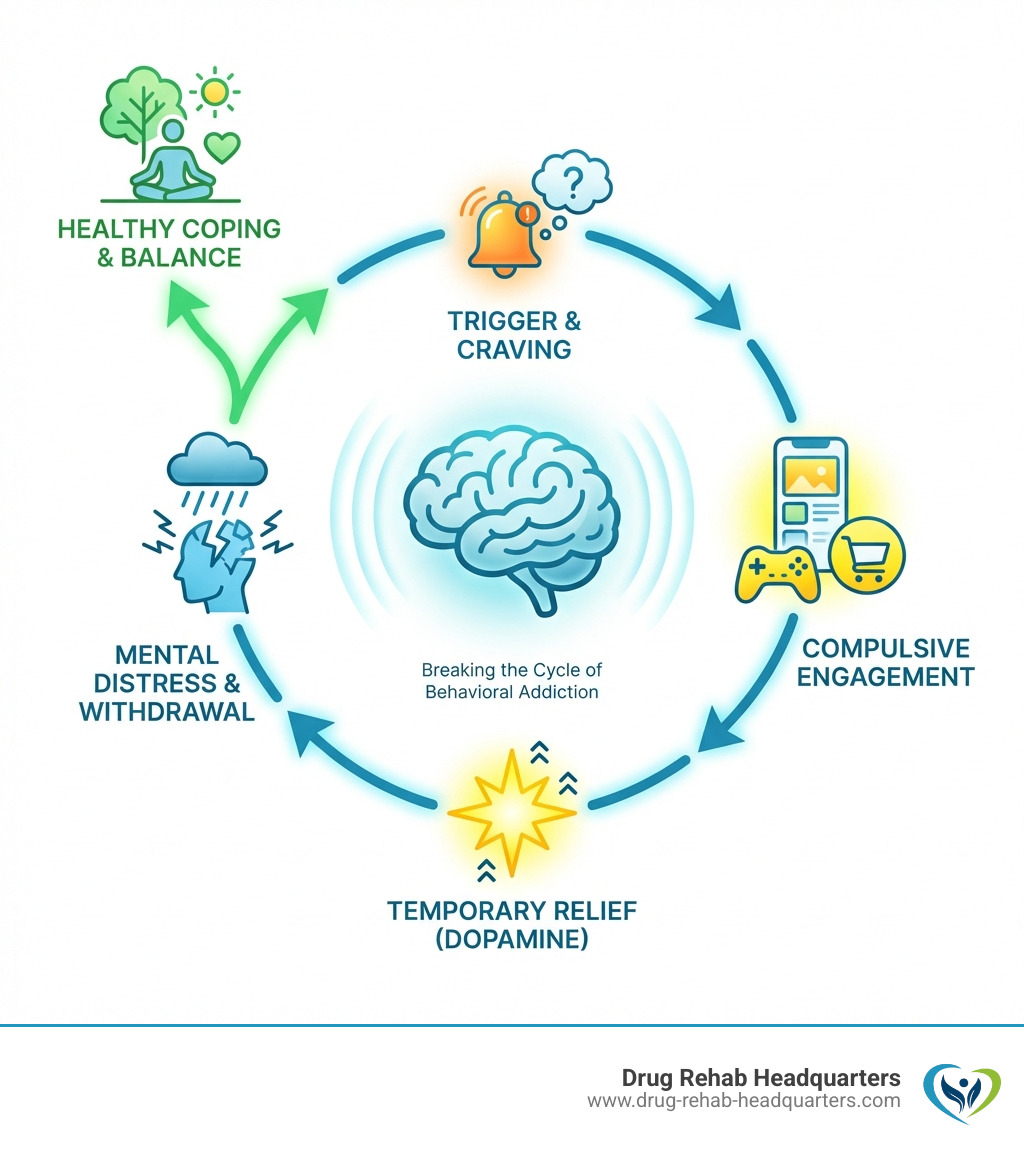
The Vicious Cycle: Why Mental Health and Addiction Intertwine
The connection between mental health conditions and addiction is deeply intertwined. It’s common for someone with a mental health diagnosis to also develop a substance use disorder, and vice versa. This complex situation is known as co-occurring disorders or dual diagnosis. As psychiatrist Ram Mahato, M.D., notes, they don’t necessarily cause each other but often fuel a vicious cycle.
Factors like stress, trauma, genetics, and brain chemistry changes contribute to this co-occurrence. A mental health condition can lead to substance use as a coping mechanism, altering brain pathways and increasing addiction risk. Conversely, substance use can change the brain, worsening mental health. This interplay demands a holistic treatment approach.
Substance use disorders are chronic brain diseases involving compulsive drug use despite negative consequences. They alter brain structure and function. When combined with a mental health condition, the challenges multiply, making effective treatment critical.
Common Risk Factors for Both Conditions
When we look at mental health addiction, we often find a shared set of vulnerabilities. Understanding these common risk factors is crucial for prevention and early intervention.
Here are some of the most common risk factors:
- Genetics and Family History: Genetics can account for 40-60% of a person’s addiction vulnerability. Many mental health conditions are also hereditary. A family history of either increases personal risk.
- Environmental Factors: Life experiences like chronic stress, poverty, lack of social support, and exposure to violence can contribute to both disorders.
- Adverse Childhood Experiences (ACEs): Traumatic childhood events like abuse, neglect, or household dysfunction are strongly linked to a higher risk of both mental health and substance use disorders later in life. This trauma can alter brain development and coping mechanisms.
- Trauma and PTSD: Significant trauma at any age (e.g., combat, accidents, assault) can lead to Post-Traumatic Stress Disorder (PTSD) and increase the risk of substance use as a coping mechanism. Effective PTSD treatment is vital for addressing co-occurring substance use.
- Early Exposure to Substances: Early substance use, especially during adolescence, increases the risk of addiction and can alter brain development, making a person more prone to mental health issues.
- Psychosocial Stressors: Ongoing stressors like job loss or relationship problems can trigger or worsen mental health conditions, leading to substance use for relief.
- Depression During or After Pregnancy: Perinatal depression is a risk factor that can affect the mother and family and may be linked to substance use.
Having these risk factors doesn’t guarantee a person will develop mental health addiction, but it highlights the importance of early intervention.
The Role of Self-Medication
Self-medication is a common link between mental health and addiction. Individuals with distressing mental health symptoms may use substances like alcohol or drugs for quick, temporary relief.
As psychiatrist Dr. Ram Mahato explains, people may use substances “to self-medicate or cope with their mental health condition.” For instance, someone with social anxiety might drink to relax, or someone with depression might use stimulants for energy. This relief is always fleeting.
The problem is that self-medication only masks underlying issues and can lead to dependence and addiction. As tolerance builds, more of the substance is needed, and stopping causes withdrawal. This cycle often worsens the original mental health symptoms and can cause new ones, creating a downward spiral as addiction leads to losses in life, such as relationships or employment.
This complex relationship shows why treating only one condition is rarely effective. An untreated mental health condition can trigger relapse, while untreated substance use can worsen mental health symptoms.
The Path to Healing: Diagnosing and Treating Mental Health Addiction
Healing from mental health addiction requires a clear diagnosis and treatment plan. Since mental health and substance use disorders can mimic or mask each other, a thorough professional assessment is crucial. Without it, treating only one condition makes lasting recovery difficult.
This complexity is why specialized care, particularly in dual diagnosis treatment facilities, is the gold standard. These facilities are equipped to handle the intricate needs of individuals with co-occurring disorders.
How Co-Occurring Disorders Are Diagnosed
Diagnosing co-occurring disorders is a nuanced process for experienced providers. The significant symptom overlap—like depression during withdrawal or anxiety leading to use—makes an accurate diagnosis key for an effective treatment plan.
A comprehensive evaluation typically involves:
- Medical History: A review of physical health, past conditions, and medications.
- Psychiatric Assessment: Interviews to understand mental health symptoms, their onset, and their impact.
- Substance Use History: An inquiry into substances used, frequency, duration, and consequences.
- Screening Tools and Questionnaires: Standardized tools to identify areas of concern.
- Observation: Professionals observe a person’s behavior, mood, and cognitive function.
Honesty with providers during diagnosis is vital. Withholding information can lead to misdiagnosis. Sharing openly is key to creating an effective plan for your healing journey. This detailed approach is a primary reason why mental health treatment centers are in high demand.
Integrated Treatment: The Gold Standard of Care
Integrated treatment is the most effective approach for mental health addiction. It means treating both the mental health and substance use disorders simultaneously, in a coordinated way, within the same program.
Older approaches treated conditions sequentially or in parallel, which proved less effective. Treating only substance use leaves underlying mental health issues unresolved, increasing relapse risk. As Dr. Mahato points out, without addressing anxiety and depression, abstinence is “much less likely.” Treating only the mental health issue while ignoring substance use is equally unstable.
Integrated care models offer several key advantages:
- Holistic View: They treat the whole person, recognizing the deep connection between the two issues.
- Coordinated Care: A multidisciplinary team works together, ensuring consistent treatment strategies.
- Improved Outcomes: Studies show integrated treatment leads to better long-term recovery rates and improved quality of life.
- Convenience: Receiving all care in one location increases engagement in treatment.
At Drug Rehab Headquarters, we connect individuals with programs that prioritize integrated care, ensuring all aspects of a person’s mental health addiction are addressed comprehensively.
Types of Therapies and Interventions
Evidence-based therapies are crucial to integrated treatment for mental health addiction. They help individuals develop coping skills, address underlying issues, and build a foundation for recovery.
Some of the most effective therapies include:
- Behavioral Therapies: These focus on changing unhealthy thought patterns and behaviors.
- Cognitive Behavioral Therapy (CBT): Helps individuals change distorted thinking patterns contributing to substance use and mental health symptoms, teaching coping strategies for triggers.
- Dialectical Behavior Therapy (DBT): Combines CBT with mindfulness, emotional regulation, and distress tolerance. It is effective for conditions like borderline personality disorder that co-occur with substance use.
- Motivational Interviewing (MI): A client-centered approach that helps individuals resolve ambivalence about change and find internal motivation, especially in early recovery.
- Family Therapy: Involves family members to improve communication, address dysfunctional patterns, and build a supportive home environment.
- Support Groups: Peer-led groups like Alcoholics Anonymous (AA) and Narcotics Anonymous (NA) provide community and shared experience. While not professional therapy, they are a vital adjunct to formal treatment.
- Coping Skills Education: Learning to manage stress, emotions, and triggers is fundamental, using techniques like mindfulness, relaxation, and problem-solving.
These therapies are adapted to specific conditions. For example, those in bipolar disorder rehab may focus on mood regulation, while those in schizophrenia treatment centers might focus on social skills and medication adherence.
The Role of Medication in Treatment
Medication is a crucial part of integrated treatment for mental health addiction. Combined with therapy, it improves recovery chances by managing withdrawal, stabilizing mood, and reducing cravings.
-
Medication-Assisted Treatment (MAT): This approach combines medication with counseling to treat substance use disorders, especially for opioids and alcohol. MAT medications can:
- Reduce Cravings: Naltrexone can reduce cravings for alcohol and opioids.
- Prevent Relapse: Buprenorphine and methadone treat opioid use disorder by reducing withdrawal and blocking other opioids, helping individuals stabilize for therapy.
- Support Detoxification: Disulfiram deters alcohol use, and acamprosate helps maintain abstinence. Nicotine replacement and varenicline are effective for tobacco addiction.
You can learn more about these options through our guide to Medication-Assisted Treatment.
-
Managing Mental Health Symptoms: Medications are also vital for treating the mental health component of a dual diagnosis.
- Antidepressants: Used to treat depression, anxiety disorders, and sometimes PTSD.
- Mood Stabilizers: Essential for managing conditions like bipolar disorder.
- Anti-anxiety Medications: Used cautiously for severe anxiety due to their dependence potential.
Medication choices are individualized by a healthcare professional. They can lessen symptoms of both disorders, providing stability for individuals to engage in therapy and build skills for long-term recovery.
Your Guide to Recovery: Finding Help and Building a Future
Taking the first step toward recovery from mental health addiction is a courageous act. It means reaching out for the support you deserve. You don’t have to walk this path alone. With the right resources and integrated treatment, a fulfilling future is possible.
How to Find Support for Mental Health Addiction
Finding the right support for co-occurring disorders is a critical step. We are here to guide you, connecting you with resources and treatment options across the country.
Here’s how you can begin to find the help you need:
- Start with Your Primary Care Provider: Your doctor can provide initial guidance and referrals to specialists.
- Seek Mental Health Professionals: Look for psychiatrists, psychologists, or therapists who specialize in dual diagnosis.
- Use Helplines and Hotlines:
- If you or someone you know is in crisis or having thoughts of suicide, call or text the 988 Suicide & Crisis Lifeline at 988, or chat at 988lifeline.org. In life-threatening situations, always call 911.
- Our certified counselors at Drug Rehab Headquarters offer 24/7 free support and can provide personalized guidance.
- Explore Online Resources and Treatment Locators:
- The Substance Abuse and Mental Health Services Administration (SAMHSA) website is a valuable resource for finding treatment.
- Our Drug Rehab Headquarters Treatment Locator can help you find programs in your area.
- For more information, explore our mental help resources section.
Seeking help is a sign of strength. We are committed to helping you find the right support for your unique situation.
Long-Term Outcomes for Mental Health Addiction Treatment
Recovery from mental health addiction is a marathon, not a sprint. The long-term outcomes for those who receive integrated treatment are promising. With sustained care, long-term success and happiness are within reach.
Here’s what individuals can expect regarding long-term outcomes:
- Improved Quality of Life: Treatment improves overall well-being, including physical and mental health. People often find a renewed sense of purpose.
- Relapse Prevention Skills: Integrated treatment provides coping strategies to manage triggers and stress without substance use. Relapse can be part of recovery; if it happens, it’s a signal to adjust the treatment plan.
- Improved Coping Strategies: Individuals learn healthier ways to process emotions and solve problems, reducing the need to self-medicate and fostering resilience.
- Stable Housing and Employment: Improved mental health and reduced substance use help individuals maintain stable housing and employment.
- Restored Relationships: Integrated treatment, including family therapy, helps heal strained relationships by improving communication and rebuilding trust.
- Ongoing Management: Recovery is an ongoing process that may involve continued therapy, medication, support groups, and healthy lifestyle choices to sustain long-term well-being.
The field of mental health addiction is constantly evolving with new research. You can explore current clinical trials on co-occurring disorders to see the latest work. These advancements offer hope for more effective interventions.
Frequently Asked Questions about Co-Occurring Disorders
It’s natural to have questions about the complexities of mental health addiction. Here, we address some common inquiries.
Which comes first: the mental illness or the addiction?
There’s no simple answer, as the relationship is complex and bidirectional. Either condition can come first, or they can emerge together.
- Mental Illness First: A mental health condition like anxiety or depression can come first, leading to substance use as a way to self-medicate. Over time, this can evolve into an addiction.
- Addiction First: Prolonged substance use can alter brain chemistry, triggering or worsening mental health conditions like depression, anxiety, or psychosis.
- Shared Risk Factors: Often, both conditions stem from shared vulnerabilities like genetics, trauma, or chronic stress. In these cases, the focus is on the shared risk factors rather than which came first.
As psychiatrist Ram Mahato, M.D., notes, one doesn’t necessarily cause the other. The key is that both interconnected conditions must be addressed, regardless of which appeared first.
Can you treat addiction without addressing the mental health issue?
Treating addiction without addressing the co-occurring mental health issue is far less effective and often leads to relapse. We strongly advise against it.
This approach is like fixing a leaky roof on a crumbling foundation—the underlying problem will eventually cause more damage. The same principle applies to mental health addiction.
- Increased Relapse Risk: Untreated mental health issues like anxiety or depression remain powerful triggers for relapse. As Dr. Mahato emphasizes, without addressing these issues, the “likelihood of them abstaining from use is much less likely.”
- Incomplete Healing: Treating only the addiction leaves suffering unaddressed. Sustainable recovery requires healing the whole person.
- Exacerbated Symptoms: An untreated mental health condition can worsen, making it harder to manage daily life and maintain sobriety.
This is why integrated treatment—addressing both disorders simultaneously—is the gold standard. It provides the best foundation for long-term recovery.
What is a dual diagnosis treatment center?
A dual diagnosis treatment facility is a specialized program for treating co-occurring mental health and substance use disorders, also known as a dual diagnosis.
These centers are effective because of their integrated approach. Instead of sequential or parallel treatment, they provide coordinated care for both conditions at once.
Key characteristics of a dual diagnosis treatment center include:
- Integrated Care Model: A unified, holistic treatment plan addresses the interconnection between the mental health condition and substance use.
- Specialized Staff: The team includes professionals trained in both mental health and addiction, such as psychiatrists, therapists, and addiction counselors.
- Comprehensive Services: Services include a range of therapies (CBT, DBT), family therapy, medication management, and psychoeducation.
- Safe and Supportive Environment: They offer a supportive environment that reduces stigma and helps individuals address all their challenges.
- Personalized Treatment Plans: Custom treatment plans are created to cater to each individual’s unique needs and recovery goals.
By offering integrated care, these centers provide the most effective path to recovery for those with mental health addiction.
Conclusion
The journey through mental health addiction is challenging but filled with hope. Mental health and substance use disorders are deeply intertwined, fueled by factors like genetics, trauma, and attempts to self-medicate.
The path to recovery involves accurate diagnosis and integrated treatment. With evidence-based therapies, medication, and support, individuals can learn coping skills, stabilize their mental health, and break free from addiction.
Recovery is a reality for many who have found the right help. You are not alone. At Drug Rehab Headquarters, we understand the complexities of mental health addiction. Our certified counselors, many with lived experience, are available 24/7 to offer free, confidential support and help you find the right inpatient drug rehab program for your needs. We connect you with holistic, evidence-based treatment options across North America for a brighter, healthier future.

