
Understanding Drug Withdrawal: The Critical First Step to Recovery
Drug withdrawal treatment is the medical and psychological care provided to manage symptoms that occur when stopping or reducing substance use after physical dependence has developed. Here’s what you need to know:
Key Components of Drug Withdrawal Treatment:
- Medical Detoxification – 24/7 monitoring and medication to manage symptoms safely
- Symptom Management – Medications like methadone, buprenorphine, or benzodiazepines to ease discomfort
- Supportive Care – Hydration, nutrition, calm environment, and emotional support
- Treatment Settings – Inpatient hospital, residential facility, or outpatient clinic based on severity
- Follow-up Care – Transition to counseling, therapy, and long-term recovery programs
When Medical Withdrawal Treatment is Necessary:
- Alcohol or benzodiazepine dependence (potentially life-threatening)
- Severe withdrawal symptoms from any substance
- History of complicated withdrawal (seizures, hallucinations)
- Co-occurring medical or mental health conditions
- Multiple previous failed attempts to quit
Drug withdrawal happens because your brain and body have adapted to the constant presence of a substance. When you suddenly remove it, your system struggles to regain balance—a process called homeostasis. This biological disruption causes withdrawal symptoms that range from uncomfortable to potentially fatal, depending on the substance.
The good news? Withdrawal is treatable. With proper medical care, medications, and support, the process becomes safer and more manageable. Research shows that short-acting opioid withdrawal typically lasts 4-10 days, while alcohol withdrawal symptoms may emerge within hours but peak around 24-72 hours. Though opioid withdrawal symptoms are seldom life-threatening, they can be uncomfortable—and without treatment, most people relapse.
At Drug Rehab Headquarters, we’ve helped thousands of individuals and families steer the complex landscape of addiction treatment, connecting them with evidence-based withdrawal management programs custom to their specific needs. Our mission is to make the path to recovery clearer and more accessible for everyone seeking help.
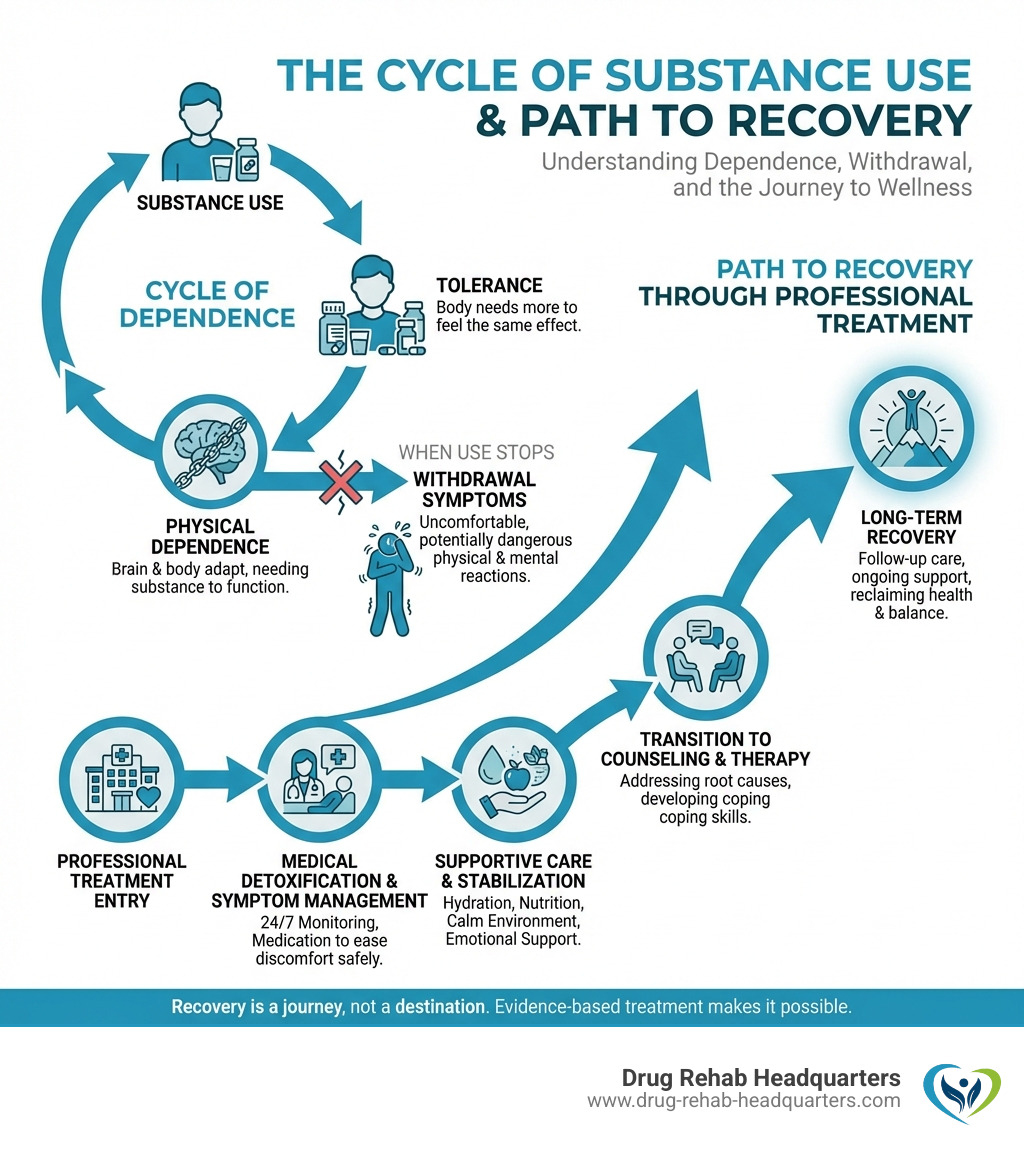
The Withdrawal Experience: Symptoms, Timelines, and Risks
When someone consistently uses a substance, their brain and body adapt to its presence. This physiological adaptation means the body becomes dependent on the substance to function “normally.” When the substance is reduced or completely stopped, the body goes into a state of imbalance, leading to a range of uncomfortable, and sometimes dangerous, symptoms. This is what we call drug withdrawal.
The severity and type of symptoms, how long they last, and the potential risks involved all vary significantly based on the substance used, the duration and amount of use, and an individual’s overall health. Understanding these differences is crucial for effective and safe drug withdrawal treatment.
Common Withdrawal Symptoms by Substance
Let’s explore some of the common symptoms associated with withdrawal from different substances:
- Opioids (Heroin, Prescription Painkillers like Oxycodone, Fentanyl): Opioid withdrawal often feels like a severe flu. Symptoms can include intense drug craving, anxiety, restlessness, muscle aches and bone pain, nausea, vomiting, diarrhea, sweating (diaphoresis), runny nose (rhinorrhea), tearing (lacrimation), yawning, and rapid heart rate (tachycardia). While rarely life-threatening, these symptoms are uncomfortable, which is why professional support during drug withdrawal treatment is so vital.
- Alcohol: Alcohol withdrawal symptoms can range from mild to severe and can be life-threatening if not managed medically. Early symptoms often include tremors, anxiety, irritability, agitation, restlessness, anorexia, nausea, vomiting, liftd heart rate and blood pressure, and insomnia. In more severe cases, hallucinations, delusions, and seizures can occur. The most dangerous form is Delirium Tremens (DTs), a severe neuro-psychiatric syndrome.
- Benzodiazepines (Xanax, Valium, Klonopin): Withdrawal from benzodiazepines can be particularly challenging and dangerous. Symptoms often include anxiety, panic attacks, severe insomnia, agitation, muscle aches, and sensory disturbances. In severe cases, hallucinations, psychosis, and life-threatening seizures can occur. Protracted withdrawal symptoms can persist for months or even years without appropriate medical intervention.
- Stimulants (Cocaine, Methamphetamine, Adderall): While often not physically dangerous in the same way as alcohol or benzodiazepine withdrawal, stimulant withdrawal can be profoundly psychologically distressing. Symptoms include intense fatigue, depression, lethargy, anxiety, unstable emotions, erratic sleep patterns (hypersomnia or insomnia), and strong cravings for the drug. This period is sometimes referred to as a “crash” followed by a protracted withdrawal phase characterized by anhedonia (inability to feel pleasure).
- Cannabis (Marijuana): Cannabis withdrawal symptoms are typically milder but can still be disruptive. They often include irritability, anxiety, restlessness, sleep disturbances (insomnia or vivid dreams), decreased appetite, and difficulty concentrating. These symptoms can last for one to two weeks.
- Inhalants: Withdrawal from inhalants can lead to symptoms like nausea, vomiting, muscle cramps, tremors, confusion, and difficulty concentrating. These symptoms can appear within hours to a few days after cessation.
How Long Does Withdrawal Last?
The duration of withdrawal is highly variable and depends on many factors, including the specific substance, how long it was used, the dosage, and individual physiology.

- Short-acting Opioids (e.g., heroin, oxycodone): Symptoms typically begin 8-24 hours after the last dose, peak within 2-4 days, and generally subside within 4-10 days.
- Long-acting Opioids (e.g., methadone): Due to their longer half-life, symptoms may not emerge for 2-4 days after the last use. The acute withdrawal phase generally fades within 10 days, though some symptoms may linger longer.
- Alcohol: Symptoms can appear within hours of the last drink, often peaking in severity over 24-72 hours. While some acute symptoms may resolve within 2-3 days, others, like Delirium Tremens, can last up to 8 days or even longer.
- Benzodiazepines: Withdrawal may begin within 1-4 days after the last use, peaking in severity in the first two weeks. However, “protracted withdrawal” symptoms, such as anxiety, insomnia, and cognitive difficulties, can remain troublesome for months or even years without specific treatment strategies.
- Stimulants: The initial “crash” phase typically lasts 3-5 days. This is often followed by a protracted withdrawal phase lasting 1-2 months, characterized by lethargy, anxiety, unstable emotions, erratic sleep patterns, and strong cravings.
- Cannabis: Symptoms usually begin within 24 hours of last use and can last between one and two weeks.
- Inhalants: Withdrawal symptoms can begin a few hours to a few days after ceasing use and typically last 2-3 days to two weeks.
When is Withdrawal Dangerous?
While all withdrawal can be uncomfortable, withdrawal from certain substances carries significant health risks, including the potential for fatality.
- Alcohol Withdrawal Risks: This is one of the most dangerous forms of withdrawal. Severe alcohol withdrawal can lead to Delirium Tremens (DTs), which is fatal in about 15% of untreated cases. DTs can manifest as profound confusion, hallucinations, severe agitation, and autonomic instability (e.g., dangerously high heart rate and blood pressure). Seizures are also a serious risk, often occurring within 7-24 hours of the last drink. Moreover, chronic alcohol use can lead to Wernicke-Korsakoff syndrome, a severe neurological disorder caused by thiamine deficiency, which can be exacerbated during withdrawal if not properly managed. For more detailed information on this serious condition, you can refer to Information on Delirium Tremens.
- Benzodiazepine Withdrawal Risks: Similar to alcohol, unmanaged benzodiazepine withdrawal can be lethal. The primary dangers include grand mal seizures and acute psychosis. The risk of these severe complications makes medically supervised withdrawal essential.
- Opioid Withdrawal Discomfort vs. Post-Detox Overdose Risk: While opioid withdrawal symptoms are uncomfortable (think severe flu-like illness), they are seldom directly life-threatening. However, the period immediately following opioid withdrawal is critically dangerous due to a significantly increased risk of overdose. After detoxification, an individual’s tolerance to opioids dramatically decreases. If they relapse and use the same amount of the drug they used before detox, it can easily lead to a fatal overdose. This highlights why detoxification is only the first step in a comprehensive drug withdrawal treatment plan, not the end of the journey.
- Stimulant Withdrawal: While generally not life-threatening, the severe depression and anhedonia experienced during stimulant withdrawal can increase the risk of suicidal ideation. Close monitoring and psychological support are crucial.
Professional Drug Withdrawal Treatment: Your Path to Safety
Given the potential dangers and severe discomfort associated with drug withdrawal, professional drug withdrawal treatment is often not just recommended, but medically necessary. This is especially true for substances like alcohol and benzodiazepines, where withdrawal can lead to seizures, Delirium Tremens, or other life-threatening complications.
When we talk about professional drug withdrawal treatment, we’re primarily referring to medical detoxification. This process provides a safe and supportive environment where medical professionals can monitor your symptoms 24/7 and administer medications to manage discomfort and prevent severe complications. The standard of care for withdrawal management emphasizes patient safety, comfort, and providing accurate information in a quiet, calm environment.
It’s important to understand the distinction between “withdrawal management” and “detoxification.” While often used interchangeably, “withdrawal management” is the preferred term in clinical settings. It refers specifically to the medical and psychological care provided during the acute withdrawal phase. “Detoxification,” on the other hand, is a broader term encompassing a set of interventions aimed at managing acute intoxication and withdrawal, ultimately clearing toxins from the body. Both aim to minimize physical harm and prepare an individual for further treatment.
Medications Used in Drug Withdrawal Treatment
Medications are a cornerstone of modern drug withdrawal treatment, helping to alleviate symptoms, prevent complications, and make the process more tolerable.
- Opioid Withdrawal Medications: Our clinical partners often use specific medications to manage opioid withdrawal:
- Methadone: A long-acting opioid agonist that can relieve withdrawal symptoms and cravings. It’s used for detox and as a long-term maintenance medicine for opioid dependence.
- Buprenorphine: A partial opioid agonist that also helps reduce withdrawal symptoms and cravings. It can shorten the length of detox and may be used for long-term maintenance. It is often combined with naloxone (Suboxone) to deter misuse.
- Clonidine: An alpha-2 adrenergic agonist that helps reduce many physical symptoms of opioid withdrawal, such as anxiety, agitation, muscle aches, sweating, and cramping. However, it does not alleviate drug cravings.
- Lofexidine: Another alpha-2 adrenergic agonist, similar to clonidine, used to reduce opioid withdrawal symptoms.
- Alcohol Withdrawal Medications: Benzodiazepines are the drugs of choice for alcohol withdrawal in inpatient settings due to their effectiveness in preventing seizures and Delirium Tremens.
- Benzodiazepines (Diazepam, Lorazepam, Chlordiazepoxide): These medications calm the central nervous system, reducing anxiety, tremors, and the risk of seizures. They are often administered on a symptom-triggered schedule, meaning doses are given based on the severity of current symptoms, which can lead to decreased total medication use and shorter treatment duration.
- Naltrexone: While not used during acute withdrawal, Naltrexone can be prescribed after detox to help prevent relapse by blocking the euphoric effects of alcohol.
- Acamprosate and Disulfiram: These medications are also used post-detox for alcohol use disorder. Acamprosate helps reduce alcohol cravings, while Disulfiram causes unpleasant reactions if alcohol is consumed.
- Benzodiazepine Taper Strategies: The safest and most effective way to manage benzodiazepine withdrawal is through a gradual reduction plan. This often involves stabilizing the patient on an equivalent dose of a long-acting benzodiazepine, like diazepam, and then slowly tapering the dosage over weeks or even months. This controlled reduction minimizes the risk of severe withdrawal symptoms, including seizures and psychosis.
- Symptom-Specific Medications: Beyond the primary medications, adjunctive medications may be used to manage specific uncomfortable symptoms during withdrawal from various substances. These can include anti-nausea medications, sleep aids, and pain relievers, used only when clinically indicated and at the minimum effective dose.
For a comprehensive understanding of detoxification and substance abuse treatment, we recommend consulting resources like the SAMHSA guide on detoxification and treatment.
Choosing the Right Level of Care
Determining the appropriate level of care for drug withdrawal treatment is a critical decision, custom to each individual’s unique needs, the severity of their dependence, and their overall health. Our certified counselors are experts in helping you steer these choices.
- Inpatient Detoxification: This is the most intensive level of care, typically provided in a hospital or specialized medical detox facility. It’s recommended for individuals with severe substance dependence, a history of complicated withdrawal (e.g., seizures, DTs), co-occurring medical or mental health conditions, or those withdrawing from substances with potentially life-threatening withdrawal symptoms (alcohol, benzodiazepines). Patients receive 24/7 medical supervision, monitoring, and medication management.
- Residential Programs: After completing acute medical detox, many individuals transition to a residential treatment program. While still providing 24/7 support in a structured environment, the focus shifts from acute medical management to therapeutic interventions and addressing the underlying causes of addiction. These programs offer a safe space for continued healing.
- Outpatient Detox: For individuals with mild to moderate withdrawal symptoms and a strong, stable support system at home, outpatient detox may be an option. This allows patients to live at home while attending regular medical appointments for monitoring and medication adjustments. However, it’s crucial that the home environment is drug-free and supportive.
- Hospitalization: In cases of severe, acute medical complications during withdrawal, such as unmanageable Delirium Tremens, severe seizures, or other critical health issues, hospitalization in a general hospital setting may be necessary. This provides immediate access to intensive medical care.
Assessing individual needs involves considering factors like the type and amount of drug used, the duration of use, the individual’s physical and mental health, and the presence of any co-occurring disorders. Our goal is to match you with the treatment option that maximizes safety, comfort, and the likelihood of successful long-term recovery. You can find more information about inpatient drug rehab options at More info about inpatient drug rehab.
Beyond Detox: Building a Foundation for Lasting Sobriety
Completing drug withdrawal treatment is a monumental achievement, a testament to your strength and commitment to change. However, it’s crucial to understand that detox is just the initial step—a critical foundation, but not the entire structure of recovery. It’s often unrealistic to expect withdrawal management alone to lead to sustained abstinence.
Statistics show us that relapse rates for substance use disorders are between 40% and 60%. This isn’t a sign of failure, but rather an indication that addiction is a chronic disease requiring ongoing care. Detoxification addresses the physical dependence, but the psychological, emotional, and behavioral aspects that drive substance use require continued attention. Without comprehensive follow-up care, individuals are at a much higher risk of returning to drug use.
The Role of Psychosocial Interventions
After the acute phase of drug withdrawal treatment is complete, psychosocial interventions become paramount. These therapies and support systems help individuals develop coping mechanisms, address underlying issues, and build a fulfilling, substance-free life.
- Individual Counseling: Therapies like Cognitive Behavioral Therapy (CBT) and Dialectical Behavior Therapy (DBT) help individuals identify and change negative thought patterns and behaviors that contribute to substance use. They also teach valuable coping skills for managing stress, cravings, and triggers.
- Group Therapy: Offers a supportive environment where individuals can share experiences, gain insights from peers, and practice new social skills. It fosters a sense of community and reduces feelings of isolation.
- Support Groups: Programs like Narcotics Anonymous (NA) and SMART Recovery provide ongoing, peer-led support. These groups emphasize personal responsibility, mutual aid, and continuous self-improvement, helping individuals maintain sobriety long-term.
- Family Therapy: Addiction impacts the entire family system. Family therapy helps heal damaged relationships, improve communication patterns, and educates family members on how to best support their loved one’s recovery journey while also addressing their own needs.
- Addressing Co-occurring Disorders: Many individuals struggling with substance use also have co-occurring mental health conditions like depression, anxiety, or PTSD. Treating these conditions simultaneously is crucial, as they often fuel each other. Integrated treatment reduces the risk of relapse and improves overall well-being. Treating co-occurring mental illnesses can significantly reduce the risk of relapse.
How Family and Friends Can Provide Support
For families and caregivers, supporting a loved one through drug withdrawal treatment and into recovery can be challenging but incredibly rewarding. Your role is vital, but it also requires self-care and healthy boundaries.
- Creating a Supportive Environment: Ensure the home environment is drug and alcohol-free. Remove any temptations and create a calm, stable atmosphere conducive to healing.
- Encouragement vs. Enabling: Understand the difference between genuine support and enabling behaviors. Encouragement empowers your loved one to take responsibility for their recovery, while enabling inadvertently perpetuates the cycle of addiction.
- Setting Healthy Boundaries: This is crucial for both your well-being and your loved one’s recovery. Boundaries protect you from burnout and hold your loved one accountable for their actions.
- Communication Strategies: Practice open, honest, and non-judgmental communication. Listen actively and express your concerns and support clearly.
- Caregiver Self-Care: Supporting someone in recovery can be emotionally draining. It’s essential to have your own support system, whether it’s through therapy, support groups for families (like Al-Anon), or simply having trusted friends to talk to. You can’t pour from an empty cup. If you need guidance on how to help someone through withdrawal, resources like Guidance on how to help someone in withdrawal offer valuable advice.
Frequently Asked Questions about Drug Withdrawal Treatment
We understand that navigating drug withdrawal treatment can bring up many questions. Here are some of the most common ones we encounter:
Can I safely detox from drugs at home?
Attempting to detox from drugs at home, especially without medical supervision, can be incredibly dangerous and is generally not recommended.
- Self-Detox Risks: For substances like alcohol and benzodiazepines, unsupervised withdrawal can lead to life-threatening complications such as seizures, Delirium Tremens, and acute psychosis. Even for substances where withdrawal isn’t typically fatal, the intense discomfort and cravings can be overwhelming, significantly increasing the risk of relapse.
- When Medical Supervision is Crucial: If you are withdrawing from alcohol or benzodiazepines, have a history of severe withdrawal symptoms (like seizures), have co-occurring medical or mental health conditions, or have been using substances heavily for a long time, medical supervision is absolutely crucial for your safety.
- Dangers of Quitting “Cold Turkey”: Abruptly stopping drug use, or “cold turkey,” can shock your system and trigger the most severe and dangerous withdrawal symptoms. This is particularly risky with central nervous system depressants.
- Importance of Consulting a Professional: We always recommend consulting with a medical professional or one of our certified counselors before attempting any form of detox. They can assess your specific situation, determine the safest course of action, and connect you with appropriate drug withdrawal treatment options.
What is the difference between detoxification and rehabilitation?
While both are integral parts of the recovery journey, detoxification and rehabilitation serve distinct purposes:
- Detoxification (Detox): This is the initial phase of drug withdrawal treatment. Its primary goal is to medically manage the acute physical symptoms of withdrawal. During detox, medical professionals monitor your vital signs, administer medications to alleviate discomfort and prevent complications, and ensure your physical stabilization. It’s about safely ridding the body of the substance and managing the immediate physiological response.
- Rehabilitation (Rehab): Following successful detox, rehabilitation focuses on the psychological, emotional, and behavioral aspects of addiction. Rehab programs, which can be inpatient or outpatient, provide comprehensive therapy, counseling, education, and support to help individuals understand the root causes of their substance use, develop coping skills, address co-occurring mental health issues, and build strategies for long-term sobriety.
- Detox as the First Stage: Think of detox as the essential first aid for addiction. It gets you physically stable. Rehab is the ongoing therapy and support that helps you heal psychologically and build a new life. Detox is rarely sufficient on its own to achieve lasting abstinence; it must be followed by comprehensive rehabilitation and ongoing support.
How do I know if I need professional withdrawal treatment?
If you’re questioning whether you need professional drug withdrawal treatment, it’s likely a sign that you do. Here are some indicators:
- Signs of Physical Dependence: You experience physical or psychological symptoms (e.g., tremors, anxiety, nausea, intense cravings) when you try to cut back on or stop using a substance.
- Inability to Quit Despite Desire: You’ve tried to stop using drugs or alcohol on your own multiple times but haven’t been successful, perhaps due to the severity of withdrawal symptoms or overwhelming cravings.
- Experiencing Withdrawal Symptoms: Any experience of withdrawal symptoms, regardless of perceived severity, warrants professional assessment. As we’ve discussed, some symptoms can escalate quickly and become dangerous.
- Impact on Daily Life: Your substance use is negatively affecting your job, relationships, health, or overall well-being, and you feel trapped in a cycle you can’t break alone.
If any of these resonate with you, it’s time to reach out. Professional help can make the process safer, more comfortable, and significantly increase your chances of achieving lasting recovery.
Conclusion
The journey to recovery begins with understanding and addressing drug withdrawal. As we’ve explored, drug withdrawal treatment is a critical, often medically necessary, step to safely steer the physical and psychological challenges that arise when the body adjusts to the absence of a substance. From managing severe, potentially lethal symptoms of alcohol and benzodiazepine withdrawal to easing the intense discomfort of opioid withdrawal, professional care makes a profound difference.
Detox is not a cure; it’s the vital first step. It clears the path for the deeper healing that occurs in rehabilitation through psychosocial interventions, counseling, and ongoing support. While the road ahead may seem daunting, with the right professional guidance and a comprehensive treatment plan, a substance-free future is not just a dream—it’s an achievable reality.
At Drug Rehab Headquarters, we believe in the power of evidence-based, holistic treatment. For personalized guidance in finding a treatment center that fits your needs across Alabama, Alaska, Arizona, Arkansas, California, Colorado, Connecticut, Delaware, Florida, Georgia, Hawaii, Idaho, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Montana, Nebraska, Nevada, New Hampshire, New Jersey, New Mexico, New York, North Carolina, North Dakota, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, South Carolina, South Dakota, Tennessee, Texas, Utah, Vermont, Virginia, Washington, West Virginia, Wisconsin, Wyoming, and Puerto Rico, we offer 24/7 free support from certified counselors, many with lived experience. Your journey starts with one step, and we’re here to help you take it.

