
When Mental Health and Addiction Collide: What You Need to Know About Dual Diagnosis Drug Detox
Dual diagnosis drug detox is the medically supervised process of safely removing substances from the body while simultaneously managing an underlying mental health condition — and it requires a very different approach than standard detox.
Here’s what that means in practice:
- Dual diagnosis = having both a substance use disorder (SUD) and a mental health condition at the same time
- Specialized detox is needed because withdrawal can trigger or worsen psychiatric symptoms like anxiety, depression, or psychosis
- Medical supervision is essential — 24/7 monitoring keeps you safe during withdrawal
- Integrated care treats both conditions at once, not one after the other
- The goal is stabilization first, then longer-term recovery through therapy and medication
If you or someone you love needs help right now, call (866) 720-3784 — support is available around the clock.
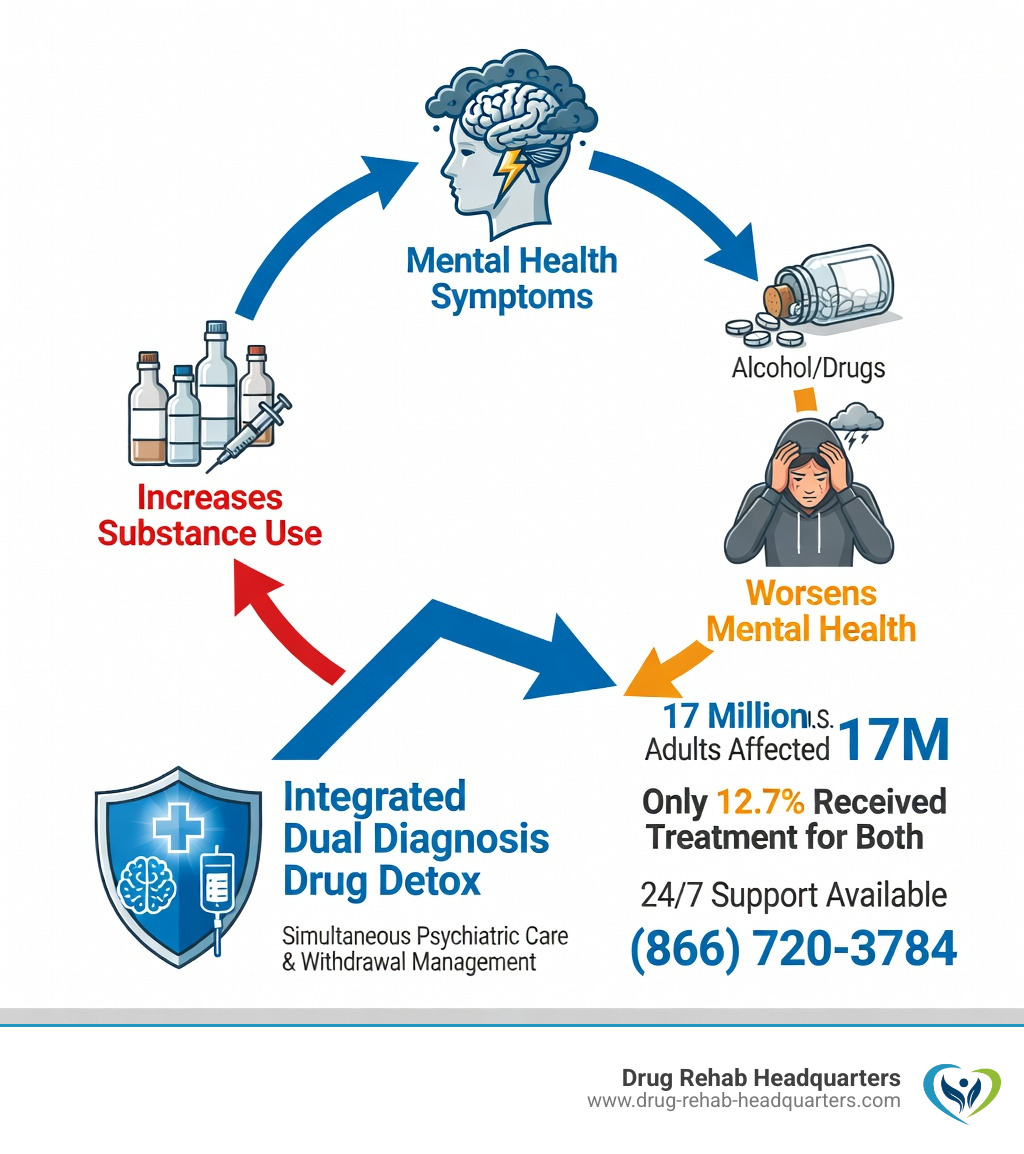
The numbers make the need painfully clear. According to SAMHSA, 17 million U.S. adults struggled with both a mental illness and a substance use disorder in 2020. Yet most standard detox programs aren’t built to handle both at once — leaving millions of people without the full care they need.
That gap can be dangerous. Detoxing without addressing an underlying mental health condition dramatically increases the risk of relapse, crisis, and incomplete recovery.
At Drug Rehabilitation Headquarters, we’ve spent years helping individuals and families find the right dual diagnosis drug detox programs — cutting through the confusion to connect people with evidence-based, integrated care. We’re here to help you do the same.
Understanding the Complexity of Dual Diagnosis Drug Detox
When we talk about dual diagnosis drug detox, we are dealing with a “chicken or the egg” scenario. Does the anxiety cause the drinking, or does the drinking cause the anxiety? Often, it’s both. This complex interplay is why a Dual Diagnosis Treatment Facility is so vital.
In the United States, around 9.2 million adults are diagnosed with co-occurring disorders. For many of these individuals, substance use began as a form of self-medication. If you feel a constant weight of depression, a pill or a drink might seem like a temporary life raft. Unfortunately, that life raft eventually springs a leak, and the substance use begins to disrupt the very brain chemistry needed to manage your mental health.
The challenge during detox is “symptom overlap.” Withdrawal from benzodiazepines can look exactly like a severe panic attack. Withdrawal from stimulants can mimic profound clinical depression. Without specialized care, it’s nearly impossible to tell where the drug effects end and the mental health condition begins. If you are confused about your symptoms, call us at (866) 720-3784 for guidance.
Common Mental Health Conditions and Addiction
Certain mental health conditions are frequently seen in dual diagnosis. According to research on most common mental health conditions, the following are high-risk pairings:
- Anxiety Disorders: Including Generalized Anxiety Disorder (GAD) and panic disorder.
- Depression: Often leading to a cycle of low energy and self-medication.
- PTSD: Trauma is a massive driver for substance use as a way to “numb” flashbacks.
- Bipolar Disorder: High-risk periods during both manic and depressive episodes.
- ADHD: Impulsivity can lead to higher rates of substance experimentation.
- Personality Disorders: Specifically Borderline Personality Disorder (BPD), which often requires specialized DBT therapy.
The Risks of Unsupervised Withdrawal
We cannot stress this enough: trying to “white-knuckle” it at home is dangerous, especially with a dual diagnosis. When you Learn about Drug Detox, you realize that withdrawal isn’t just uncomfortable; it can be life-threatening.
For those with co-occurring disorders, the risks include:
- Seizures and DTs: Common in severe alcohol or benzo withdrawal.
- Psychosis: A sudden break from reality that is much harder to manage if you already struggle with a condition like schizophrenia or bipolar disorder.
- Suicidal Ideation: The “crash” after stopping drugs can lead to dark thoughts. If you have a history of depression, this risk is amplified.
If you are experiencing a medical emergency, call 911. For help finding a safe place to land, call (866) 720-3784.
The Specialized Process of Medical Stabilization
The first step in any dual diagnosis drug detox is stabilization. This isn’t just about getting the drugs out of your system; it’s about making sure your mind and body don’t go into shock during the process. Most Medical Detox Programs last between 3 and 7 days, though this can vary depending on the substance and the severity of the mental health symptoms.
During this window, we focus on 24-hour monitoring. We aren’t just checking your blood pressure; we’re checking your “emotional vitals” too. Are you becoming increasingly paranoid? Is your depression deepening? Our clinical teams are trained to spot these shifts before they become a crisis.
The Role of Medical Supervision in Dual Diagnosis Drug Detox
In a Detox Treatment setting, medical supervision serves as your safety net. This involves:
- Constant Vitals Monitoring: Keeping an eye on heart rate and temperature.
- Psychiatric Evaluation: Meeting with a psychiatrist early in the process to adjust or maintain mental health medications.
- Safety Protocols: Ensuring the environment is “trigger-free” and secure.
- Withdrawal Management: Using specialized tools like the CIWA scale for alcohol or the COWS scale for opioids to measure exactly how much help your body needs.
If you’re worried about the cost or location of these programs, our team at (866) 720-3784 can help you find a facility in states like Illinois, California, New York, or any of the 50 states we serve.
Medications Used in Dual Diagnosis Care
One of the biggest myths in recovery is that you have to be “100% medication-free” to be sober. In dual diagnosis, Certain medications are actually the keys to the kingdom.
We utilize Medication-Assisted Treatment (MAT) to ease the transition:
- Suboxone or Methadone: For opioid withdrawal.
- Acamprosate or Naltrexone: To reduce alcohol cravings.
- Psychiatric Stabilizers: Continuing (or starting) antidepressants or anti-anxiety meds that won’t interfere with the detox process.
The goal isn’t to replace one drug with another; it’s to use medicine as a tool to keep you stable enough to actually participate in therapy. Questions about MAT? Call us at (866) 720-3784.
Integrated Therapies and Medication Management
Once the physical “fog” of detox begins to lift, the real work of Integrated Healing: Co-Occurring Disorder Treatment begins. We don’t wait until you are 30 days sober to talk about your depression. We start as soon as you are medically stable.
Integrated care means your therapist and your doctor are talking to each other. If your anxiety spikes during a therapy session, your medical team is alerted. This holistic approach ensures that no part of your health is ignored.
Evidence-Based Behavioral Therapies
We rely on therapies that have been scientifically proven to help people with dual diagnosis. Why Treatment for PTSD is Beyond Important becomes clear when you see how trauma-informed care can prevent a relapse.
Common therapies include:
- CBT (Cognitive Behavioral Therapy): Helping you identify the “stinking thinking” that leads to drug use.
- DBT (Dialectical Behavior Therapy): Vital for emotional regulation and managing suicidal thoughts.
- EMDR (Eye Movement Desensitization and Reprocessing): A powerful tool for processing trauma without having to “relive” it verbally for hours.
Peer Support and Long-Term Stability
You are not alone in this. Millions of people have walked this path before you. Organizations like Dual Diagnosis Anonymous provide a space where you don’t have to hide your mental health diagnosis to talk about your addiction.
Whether it’s a traditional 12-step program or a secular alternative like SMART Recovery, finding a tribe of people with “lived experience” is one of the best predictors of long-term success. Our counselors at (866) 720-3784 can help you find local meetings in your community.
Navigating Levels of Care and Insurance
Choosing the right level of care is like choosing the right medicine — it has to be the right dose for your specific situation.
| Level of Care | Hours of Care | Best For… |
|---|---|---|
| Inpatient/Residential | 24/7 | Severe addiction + unstable mental health |
| PHP (Partial Hospitalization) | 5-6 hours/day | Those needing structure but have a safe home |
| IOP (Intensive Outpatient) | 9-15 hours/week | Transitioning back to work/life |
Before you commit, it is vital to Verify Your Insurance. Thanks to the Mental Health Parity and Addiction Equity Act, most insurance plans are required to cover dual diagnosis treatment just as they would any other medical condition. Call us at (866) 720-3784 and we can do the heavy lifting of checking your benefits for you.
Inpatient vs. Outpatient Dual Diagnosis Drug Detox
For most people starting dual diagnosis drug detox, we recommend Inpatient Drug Rehab. Why? Because the risk of a mental health crisis is highest in the first 72 hours.
Inpatient care provides:
- A “Bubble” of Safety: No access to substances.
- Immediate Crisis Intervention: If you have a panic attack at 3 AM, someone is there.
- Clinical Supervision: Constant adjustments to your care plan.
Outpatient detox is sometimes an option for very mild cases, but it requires a rock-solid support system and a very low risk of psychiatric emergency.
Transitioning After Dual Diagnosis Drug Detox
Detox is the “reset” button, but it isn’t the whole game. To stay sober, you need a plan for what happens next. This usually involves stepping down to a PHP or IOP program and eventually finding a sober living environment.
You can use the SAMHSA Treatment Locator to find options, or you can call us at (866) 720-3784 for a more personalized recommendation based on our database of vetted facilities across North America.
Frequently Asked Questions
What is the difference between dual diagnosis and co-occurring disorders?
In the clinical world, they are essentially the same thing. “Dual diagnosis” is the more traditional term, while “co-occurring disorders” (COD) is the preferred term used by organizations like SAMHSA. Both refer to having a mental health condition and a substance use disorder simultaneously.
How long does the dual diagnosis detox process typically last?
For most, the acute phase of dual diagnosis drug detox lasts 3 to 7 days. However, because we are also stabilizing mental health medications, some people may stay in a clinical detox setting for up to 10 or 14 days to ensure they are emotionally “level” before moving to the next stage of rehabilitation.
Does insurance cover specialized dual diagnosis treatment?
Yes! Under the Affordable Care Act (ACA), mental health and substance abuse services are considered “essential health benefits.” This means your insurance provider cannot deny you coverage just because you have a dual diagnosis. We can help you verify your specific coverage at (866) 720-3784.
Conclusion
Navigating dual diagnosis drug detox can feel like trying to solve a puzzle in the dark. But you don’t have to do it alone. At Drug Rehabilitation Headquarters, we are dedicated to connecting you with the care that addresses all of you — not just your addiction.
Our 24/7 free support line is staffed by certified counselors, many of whom have been exactly where you are right now. We offer personalized guidance to find evidence-based, holistic treatment options in every state from Alabama to Wyoming.
The cycle of self-medication and mental health struggles can be broken. It starts with a single, safe step. Start your recovery journey today and give us a call at (866) 720-3784. We’re ready when you are.
Types of Rehab Centers in Indiana
Indiana offers a variety of facilities tailored to co-occurring disorders, including specialized drug rehab centers that focus on integrated psychiatric care. The cost of these programs in Indiana can vary; outpatient services typically range from $2,000 to $8,000, while comprehensive residential programs may cost between $15,000 and $45,000 depending on the level of medical supervision required.
Inpatient vs. Outpatient Treatment in Indiana
When deciding between inpatient rehab and outpatient care in Indiana, patients must consider the intensity of their mental health symptoms. Inpatient treatment provides a secure environment for those at high risk of psychiatric crisis during withdrawal, whereas outpatient treatment is suitable for individuals with stable living environments and milder symptoms.
Finding the Right Addiction Treatment Program
Selecting the right program involves evaluating clinical expertise in both addiction and mental health. Success rates for individuals with co-occurring disorders are significantly higher when they receive integrated treatment. Studies show that patients in integrated programs are twice as likely to maintain long-term sobriety compared to those receiving sequential treatment.
Insurance Coverage for Indiana Rehab Centers
Understanding Insurance Coverage for Indiana Rehab Centers is essential for accessing care. Most Indiana residents are covered by providers like Anthem, CareSource, or Managed Health Services, which are required by law to provide benefits for mental health and substance use disorders. Our team can help you navigate these benefits to ensure your rehabilitation is covered with minimal out-of-pocket expenses.

