
Understanding the Critical Connection Between Mental Health and Addiction
Co-occurring disorder treatment addresses the simultaneous presence of both a mental health condition and a substance use disorder. When you or a loved one faces both challenges at once, you need integrated care that treats both conditions together—not separately. Here’s what you need to know:
Key Facts About Co-Occurring Disorder Treatment:
- What it is: Specialized care that addresses mental health disorders (like depression, anxiety, PTSD) and substance use disorders at the same time, with the same treatment team
- Why it matters: About 9.5 million adults in the U.S. have both conditions, and more than 50% never receive treatment for either disorder
- The gold standard: Integrated treatment—where both conditions are treated simultaneously—leads to better outcomes than treating them separately
- Common settings: Inpatient rehab, outpatient programs, partial hospitalization, and intensive outpatient care
- Coverage: The Affordable Care Act requires most insurance plans to cover treatment for both mental health and substance use disorders
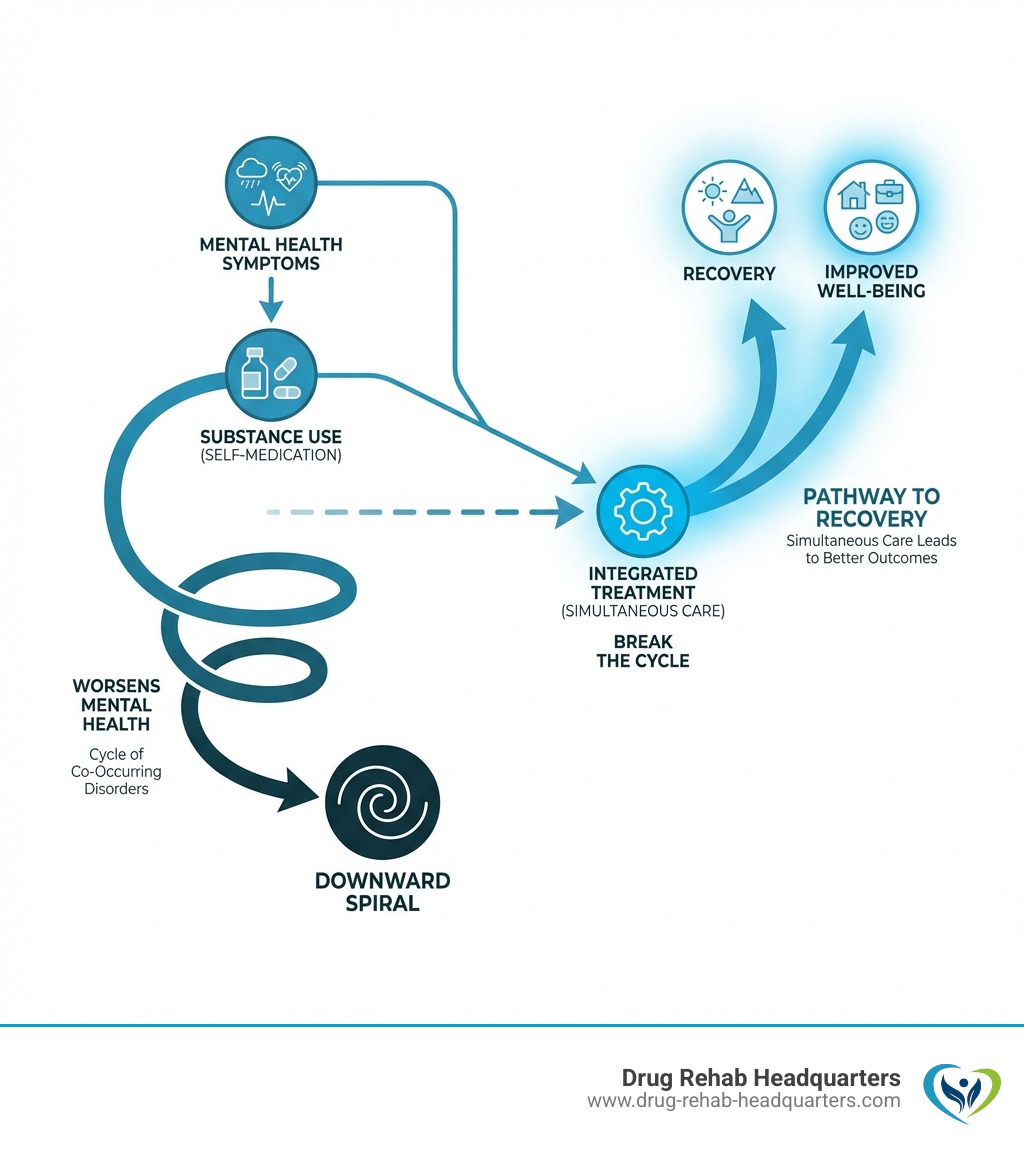
The reality is stark: when mental health conditions and addiction occur together, they create a dangerous cycle. Each condition can worsen the other. Someone struggling with depression might turn to alcohol for relief, but the alcohol deepens the depression. A person with anxiety might use drugs to calm their nerves, only to find their anxiety intensifies during withdrawal.
The good news? Recovery is absolutely possible when both conditions receive proper attention at the same time. Research shows that people who receive integrated treatment are more likely to stay sober, experience significant symptom reduction, maintain stable housing, keep steady employment, and report greater life satisfaction.
At Drug Rehab Headquarters, we specialize in connecting individuals and families with treatment centers that provide integrated co-occurring disorder treatment, helping you find programs that address both mental health and addiction simultaneously. Our team understands the unique challenges of dual diagnosis and works to match you with evidence-based care custom to your specific needs.
Key Co-occurring disorder treatment vocabulary:
- addiction recovery treatment centers
- addiction recovery centers arizona
- addiction recovery centers in kentucky
Understanding Co-Occurring Disorders: When Two Paths Collide
When we talk about co-occurring disorders, we’re referring to the presence of both a mental health condition and a substance use disorder (SUD) at the same time. This is also commonly known as a “dual diagnosis.” While the terms “dual diagnosis” and “co-occurring disorders” are often used interchangeably, “co-occurring disorders” is increasingly preferred in clinical settings to emphasize that these are two distinct, yet interconnected, conditions requiring simultaneous attention. “Comorbidity” is a broader medical term for co-existing conditions, which can apply to any two or more illnesses, not just mental health and substance use.
The prevalence of co-occurring disorders is significant. According to recent data, of the 20.3 million adults diagnosed with SUDs, more than a third also suffer from a mental illness. Conversely, almost 20% of the 42.1 million people diagnosed with a mental health condition also have a SUD. These statistics highlight a critical public health challenge, as more than 50% of those diagnosed with co-occurring disorders never receive treatment for either condition.
Why do these conditions often appear together? The relationship is complex and often bidirectional.
- Self-Medication Hypothesis: Many individuals with mental health conditions may turn to substances as a way to cope with their symptoms. For example, someone with anxiety might use alcohol to calm their nerves, or someone with depression might use stimulants to boost their mood. While this might offer temporary relief, it ultimately worsens both conditions.
- Shared Risk Factors: There are overlapping environmental factors, genetics, and brain vulnerabilities that can predispose individuals to both mental disorders and SUDs. Trauma, chronic stress, and a family history of either condition can increase the risk for both.
- Brain Changes: Substance use can cause changes in brain chemistry and structure that mimic or exacerbate mental health disorders, making individuals more susceptible to developing a mental illness or worsening an existing one.
Understanding this intricate connection is the first step toward effective co-occurring disorder treatment. For more information on navigating mental health challenges, you can explore resources on mental help. We also encourage you to dig into the scientific research on Co-Occurring Disorders and Health Conditions.
Common Co-Occurring Mental Health Conditions
While any mental health condition can co-occur with a substance use disorder, some are more commonly observed. Recognizing these can help us identify potential dual diagnoses earlier:
- Anxiety Disorders: Approximately 18% of the general population has a co-occurring anxiety disorder of some type. People often use substances to alleviate anxiety symptoms, but this can lead to dependence and worsen anxiety in the long run. If you’re struggling with anxiety, understanding anxiety disorder treatment information can be very helpful.
- Mood Disorders: About 20% of the general population with a SUD also have one or more mood disorders, such as bipolar disorder or depression.
- Depression: Often characterized by persistent sadness, loss of interest, and low energy. Individuals may use substances to escape depressive feelings, but this can deepen their depression and complicate treatment. For insights into managing depression, consider exploring depression treatment.
- Bipolar Disorder: Involves extreme mood swings, from manic highs to depressive lows. The impulsivity associated with manic episodes can increase the likelihood of substance use, while substances can destabilize mood. For those dealing with both, bipolar disorder and addiction information is crucial.
- Post-Traumatic Stress Disorder (PTSD): People with PTSD were as much as 4 times more likely to also meet criteria for a substance use disorder. They may use substances to numb painful memories or to help them sleep, creating a cycle of addiction and trauma.
- Personality Disorders: In the normal population, approximately 10-15% have a personality disorder, compared to a prevalence rate of about 35-73% in patients treated for addiction. These disorders, such as Borderline Personality Disorder, can involve intense emotional dysregulation and impulsive behaviors that contribute to substance use.
- Schizophrenia and Other Psychotic Disorders: About 25% of people with severe mental illness develop co-occurring disorders. Individuals with schizophrenia may use substances to cope with distressing symptoms or medication side effects. For more on this, consider resources on schizophrenia treatment centers.
- Attention-Deficit/Hyperactivity Disorder (ADHD): ADHD is associated with an earlier age at onset of substance use and a higher likelihood of using a variety of substances. Individuals may use stimulants to self-medicate or other substances to calm hyperactivity or aid sleep.
Recognizing the Signs and Symptoms
Recognizing the signs and symptoms of co-occurring disorders can be challenging because the symptoms of mental health conditions and substance use disorders often overlap or mimic each other. It can be difficult to tell where one ends and the other begins, especially during periods of intoxication or withdrawal.

However, some common indicators that might suggest a co-occurring disorder include:
- Sudden Behavioral Changes: Unexplained shifts in mood, energy levels, sleep patterns, or social interactions.
- Difficulty Managing Daily Tasks: Struggling with work, school, relationships, or personal hygiene beyond what might be expected from one condition alone.
- Social Withdrawal: Isolating from friends, family, and activities once enjoyed.
- Worsening Mental Health Despite Treatment: If a mental health condition doesn’t improve with therapy or medication, or if addiction treatment isn’t effective, it could indicate an underlying, untreated co-occurring disorder.
- Using Substances to Cope: Regularly using drugs or alcohol to manage feelings of anxiety, depression, stress, or trauma.
- Increased Risk-Taking Behavior: Engaging in dangerous activities due to impaired judgment from both conditions.
A thorough and professional assessment is crucial to accurately diagnose both conditions. In some cases, an assessment may even be conducted after a period of abstinence to differentiate between symptoms caused by substance use and those indicative of a mental health disorder.
How Co-Occurring Disorders Impact Recovery
The presence of co-occurring disorders significantly complicates the path to recovery for both conditions. Dual diagnosis is associated with a variety of negative outcomes, making recovery more challenging without integrated care:
- Higher Rates of Relapse: When one disorder is left untreated, it often triggers the other, leading to a higher likelihood of returning to substance use or experiencing a resurgence of mental health symptoms.
- Increased Hospitalization Risk: Individuals with co-occurring disorders are more prone to psychiatric crises and medical emergencies, often requiring more frequent hospitalizations.
- Homelessness and Incarceration: The instability caused by untreated co-occurring disorders can lead to housing insecurity and increased involvement with the criminal justice system.
- Compounded Health Problems: The physical and mental health consequences of both conditions can combine, leading to more severe health issues and a reduced quality of life.
- Social and Functional Impairment: Daily functioning, relationships, and employment can be severely impacted, making it difficult to maintain stability.
These negative outcomes underscore the critical importance of addressing both conditions simultaneously. Treating only one disorder while ignoring the other is often ineffective and can perpetuate a cycle of suffering.
The Gold Standard: Why Integrated Treatment is Essential
Integrated treatment is not just a preference; it’s considered the gold standard for individuals with co-occurring disorders. This approach means that both the mental health condition and the substance use disorder are treated concurrently by the same team of healthcare professionals, ideally within the same treatment setting.
The diagnostic process for co-occurring disorders is comprehensive. It involves a thorough assessment by experienced healthcare providers who are trained in both mental health and substance use. They use a range of tools and interviews to gather information about an individual’s history, symptoms, substance use patterns, and overall functioning. This comprehensive assessment is vital because, as we mentioned, symptoms can overlap, making accurate diagnosis tricky. Sometimes, an initial period of medically supervised detoxification may be necessary to stabilize the individual before a precise mental health diagnosis can be made, as withdrawal symptoms can mimic mental health issues.
A key principle in effective co-occurring disorder treatment is the “no wrong door” policy. This means that no matter if an individual first seeks help for their mental health or their substance use, the treatment system should be equipped to identify, assess, and provide or refer them to appropriate care for both conditions. This ensures that individuals aren’t turned away or forced to steer complex, separate systems, which historically has been a significant barrier to effective care.

Integrated care addresses both disorders as primary, interconnected issues. Instead of sequential treatment (treating one after the other), or parallel treatment (treating both separately by different providers), integrated care combines interventions into one coherent, coordinated package. This seamless approach makes the treatment process less confusing and more effective for the individual.
The Proven Benefits of an Integrated Approach
The evidence is clear: integrated treatment leads to significantly better outcomes for individuals with co-occurring disorders. Studies consistently show that this approach offers a multitude of benefits, paving the way for more stable and lasting recovery.
Individuals who receive integrated co-occurring disorder treatment are more likely to experience:
- Reduced Substance Use or Sustained Sobriety: By addressing the underlying mental health issues that often fuel substance use, individuals are better equipped to manage cravings and maintain abstinence.
- Improved Psychiatric Symptoms: When substance use is controlled, mental health medications and therapies become more effective, leading to a significant reduction in symptoms like anxiety, depression, or psychosis.
- Better Quality of Life: With both conditions managed, individuals report feeling happier with their lives, experiencing greater overall well-being, and having the capacity to pursue personal goals.
- Increased Housing Stability: Addressing both mental health and substance use helps individuals maintain stable living situations, reducing instances of homelessness.
- Fewer Arrests: Improved decision-making and reduced impulsive behaviors often lead to less involvement with the criminal justice system.
- Higher Treatment Retention: Integrated programs are designed to be more engaging and supportive, leading to higher rates of patients staying in treatment longer.
- Decreased Hospitalization: Better management of both conditions means fewer crises and less need for emergency room visits or inpatient psychiatric admissions.
- Reduced Medication Interactions: A single, coordinated team can better manage medications for both conditions, reducing the risk of adverse interactions.
These benefits highlight why integrated care is not just a compassionate approach, but a highly effective one. For more information about the specifics of this treatment model, we encourage you to explore our resources on dual diagnosis treatment.
The Problem with Separate Treatment
Historically, mental health and substance use treatment systems developed independently, leading to a fragmented approach to care. This separation has created significant barriers and often resulted in ineffective outcomes for individuals with co-occurring disorders.
When mental health and substance use are treated separately:
- Fragmented Care: Individuals often receive conflicting advice, different medications, and uncoordinated care from multiple providers who may not communicate with each other. This can be confusing and overwhelming.
- Lack of Communication: Mental health providers might not be trained in substance use, and addiction specialists might lack expertise in mental health. This lack of integrated knowledge means critical information about a patient’s overall condition can be missed.
- Higher Dropout Rates: Navigating two separate treatment systems can be exhausting and discouraging. Patients may feel misunderstood or that their unique needs are not being met, leading them to drop out of one or both programs.
- Ineffective Outcomes: Treating only one condition often leads to the other condition worsening or triggering a relapse. For example, treating depression without addressing co-occurring alcohol use might fail because alcohol can negate the effects of antidepressants and exacerbate depressive symptoms.
- “Wrong Door” Scenario: If a person seeks help for depression but isn’t screened for substance use, they might be placed in a mental health program that isn’t equipped to handle their addiction, leading to frustration and continued suffering.
The shift towards integrated co-occurring disorder treatment recognizes these historical shortcomings and seeks to provide a more holistic, person-centered, and ultimately more successful path to recovery.
Comprehensive Co-occurring Disorder Treatment Approaches
Effective co-occurring disorder treatment demands a comprehensive and individualized approach. There’s no one-size-fits-all solution, as each person’s unique combination of conditions, life experiences, and treatment needs must be carefully considered. The goal is to provide a continuum of care that addresses both disorders at every stage, leveraging evidence-based practices for the best possible outcomes.
The treatment plan should be dynamic, adapting as an individual progresses through different stages of recovery. It often combines various therapeutic modalities, medication management, and supportive services, all aimed at fostering long-term well-being. For a deeper dive into general addiction treatment, you can find more information on addiction treatment.
What Does an Integrated Co-occurring Disorder Treatment Plan Involve?
An integrated treatment plan typically involves a combination of therapies and, when appropriate, medication, all delivered in a coordinated manner.
Behavioral Therapies: These are cornerstones of co-occurring disorder treatment, helping individuals develop coping skills, modify harmful behaviors, and address underlying thought patterns.
- Cognitive Behavioral Therapy (CBT): Helps individuals identify and change negative thought patterns and behaviors that contribute to both substance use and mental health symptoms. It teaches strategies for managing stress, triggers, and cravings.
- Dialectical Behavior Therapy (DBT): Often used for individuals with severe emotional dysregulation, such as those with Borderline Personality Disorder or chronic suicidal ideation. DBT focuses on mindfulness, distress tolerance, emotion regulation, and interpersonal effectiveness.
- Motivational Interviewing (MI): A client-centered approach that helps individuals explore and resolve their ambivalence about change, strengthening their motivation to engage in treatment and recovery.
- Contingency Management (CM): Uses positive reinforcement (e.g., vouchers or small rewards) to encourage desired behaviors, such as abstinence from substances or adherence to treatment goals.
Medication Management: Medications can be a vital component of integrated treatment, especially for managing symptoms of mental health conditions and reducing cravings or withdrawal symptoms associated with SUDs.
- Antidepressants can help stabilize mood for individuals with depression or anxiety.
- Mood stabilizers are crucial for managing bipolar disorder.
- Anti-anxiety medications may be used short-term, with careful monitoring.
- Medications for Opioid Use Disorder (MOUD), such as buprenorphine or naltrexone, can significantly aid recovery from opioid addiction. Similarly, medications like naltrexone or acamprosate can support recovery from alcohol use disorder.
- Bupropion (Wellbutrin®, Zyban®) is an example of a medication approved to treat depression and nicotine dependence, demonstrating how some medications can address aspects of co-occurring conditions.
It’s important that medication management is closely monitored by healthcare professionals experienced in both mental health and addiction to ensure safety and effectiveness. For detailed information on medications for opioid use disorder, you can refer to the FDA’s Information about Medications for Opioid Use Disorder (MOUD). Additionally, if you’re seeking to understand treatment options for depression, we have more information on depression treatment.
Levels of Care: Finding the Right Treatment Setting
The journey through co-occurring disorder treatment often involves different levels of care, custom to the severity of both the mental health condition and the substance use disorder. The goal is to provide the most appropriate and least restrictive environment necessary for effective treatment and safety.
| Level of Care | Description |
|---|---|
| Detoxification (Detox) | Medically supervised withdrawal to manage physical symptoms and ensure safety before starting formal treatment. |
| Inpatient/Residential Rehab | 24/7 care in a structured, live-in facility. Offers intensive therapy, medical supervision, and a supportive environment away from triggers. |
| Partial Hospitalization Program (PHP) | A highly structured program with daily treatment (several hours a day, 5-7 days a week) while the individual lives at home or in sober living. |
| Intensive Outpatient Program (IOP) | A step down from PHP, offering treatment for a few hours a day, several days a week. Allows individuals to maintain work or school commitments. |
| Standard Outpatient | Less intensive than IOP, involving weekly therapy sessions (individual or group) to support ongoing recovery. |
| Aftercare Planning | Continued support after formal treatment ends. Includes ongoing therapy, support groups, and relapse prevention strategies to maintain long-term recovery. |
