
Why DBT for Addiction Offers Hope Beyond Traditional Therapy
DBT for addiction is a skills-based therapy that teaches people struggling with substance use how to manage intense emotions, tolerate distress, and build a life worth living without drugs or alcohol. Here’s what makes it different:
- Balances acceptance and change – DBT helps you accept your current situation while learning new skills to create change.
- Addresses root causes – It targets the emotional dysregulation and impulsivity that often drive substance use.
- Proven results – Studies show 87.5% of participants achieved remission with DBT, compared to only 33.3% in standard treatment.
- Treats co-occurring issues – It’s effective for addiction alongside depression, anxiety, trauma, and eating disorders.
- Multiple support formats – Includes individual therapy, group skills training, and phone coaching for real-time help.
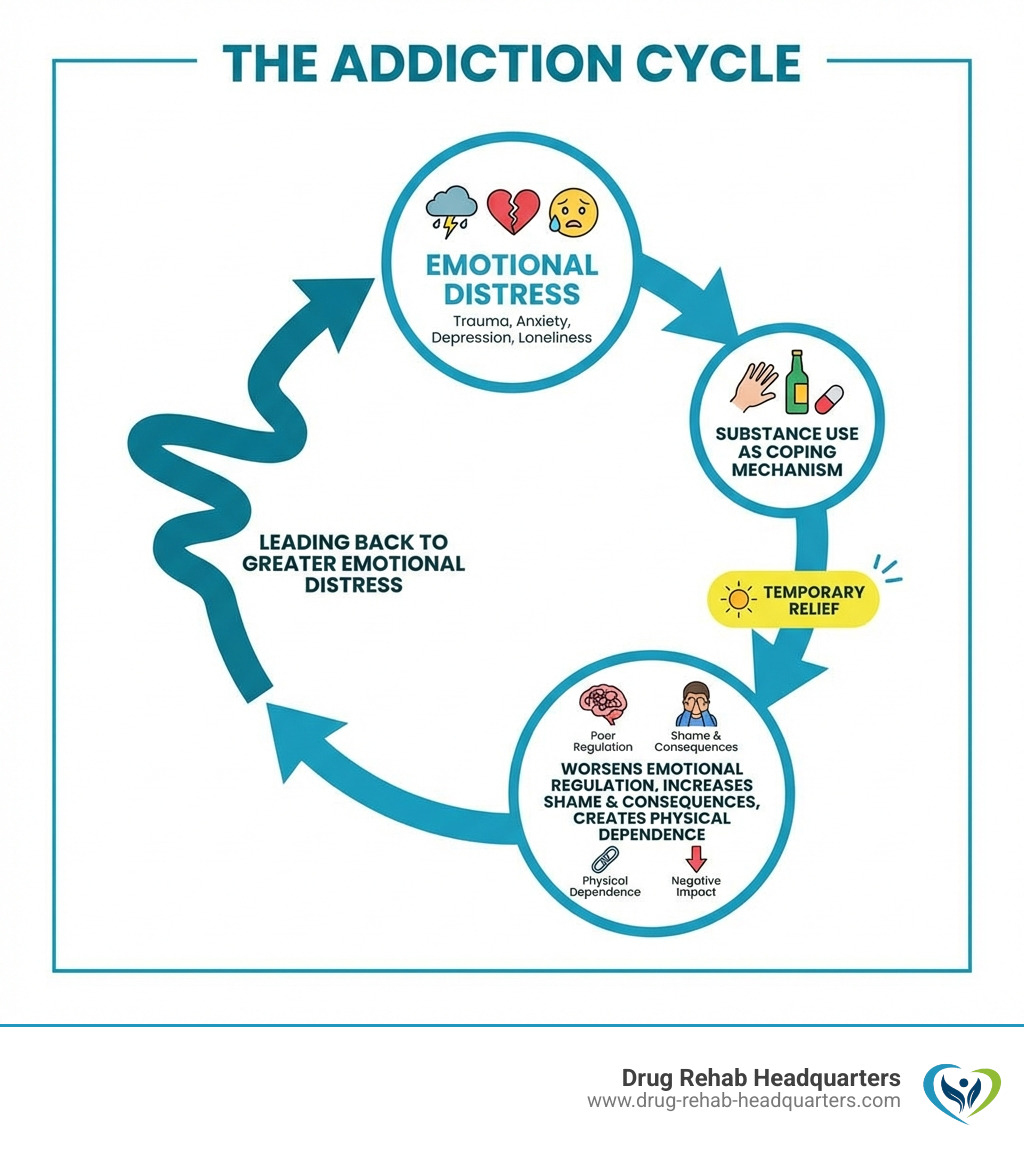
Millions of Americans struggle with substance use disorders that stem from an inability to cope with emotional pain. When anxiety, depression, or trauma become unbearable, drugs and alcohol can feel like the only escape. This creates a devastating cycle: substance use provides temporary relief but ultimately worsens the distress, leading to more use.
DBT breaks this cycle by teaching practical skills in four key areas: mindfulness (staying present), distress tolerance (getting through crises without substances), emotion regulation (managing feelings effectively), and interpersonal effectiveness (building healthy relationships). Research shows these skills can dramatically reduce substance abuse and improve overall quality of life.
At Drug Rehab Headquarters, we help people integrate DBT into comprehensive treatment. Our experience shows that these skills help people not just stop using substances, but build lives they don’t want to escape from.
Understanding Dialectical Behavior Therapy (DBT) and Its Core Principles
Dialectical Behavior Therapy (DBT) is a guide of hope for complex mental health challenges. Developed by Dr. Marsha Linehan, DBT was initially designed for individuals with Borderline Personality Disorder (BPD) who experienced intense emotional pain and lacked coping skills. Today, its applications are much broader.
The core of DBT is its “dialectical” philosophy—the idea of balancing opposites. It teaches the acceptance of ourselves as we are, while simultaneously working to change and grow. This balance is powerful for those navigating addiction, as it acknowledges struggles without judgment while committing to building healthier responses to life’s challenges.
DBT is a “third-wave” behavioral therapy, incorporating mindfulness into its approach. It’s grounded in the biosocial theory, which suggests emotional dysregulation comes from a biological predisposition combined with an invalidating environment. This allows for a compassionate, skill-building approach rather than blame.

What is DBT and How Does It Differ from CBT?
Many people are familiar with Cognitive Behavioral Therapy (CBT), which focuses on changing unhelpful thought patterns. DBT stems from CBT but adds a crucial emphasis on validation and acceptance. Before changing uncomfortable thoughts or feelings, DBT teaches us to first accept them without judgment. This validation is vital for individuals with histories of feeling criticized or dismissed.
The key differentiator is the “dialectical” philosophy. While CBT focuses primarily on change, DBT balances acceptance and change. This blend helps address the deep-seated emotional dysregulation that often fuels addiction.
As a “third-wave” therapy, like Acceptance and Commitment Therapy (ACT), DBT focuses on changing our relationship with our thoughts and feelings rather than just their content. These therapies aim to disrupt cycles of avoiding internal pain by fostering acceptance and mindfulness. This is why scientific research on third-wave behavioral therapies highlights their promise for treating conditions like substance use disorders.
Here’s a quick comparison:
| Feature | Cognitive Behavioral Therapy (CBT) | Dialectical Behavior Therapy (DBT) |
|---|---|---|
| Core Focus | Changing maladaptive thoughts and behaviors. | Balancing acceptance of self/situation with the need for change; building a life worth living. |
| Primary Goal | Symptom reduction, cognitive restructuring. | Emotional regulation, distress tolerance, interpersonal effectiveness, mindfulness, reducing self-destructive behaviors. |
| Key Strategies | Cognitive restructuring, behavioral experiments, exposure therapy. | Validation, dialectical strategies, behavioral chain analysis, skills training (mindfulness, distress tolerance, emotion regulation, interpersonal effectiveness), phone coaching, therapist consultation team. |
| Emotional Approach | Identifies and challenges irrational or unhelpful thoughts. | Validates emotional experiences first, then teaches skills to manage and regulate them. Focuses on accepting feelings without necessarily acting on them. |
| Therapy Structure | Primarily individual therapy, sometimes group. | Comprehensive program including individual therapy, weekly group skills training, phone coaching, and a therapist consultation team. |
| Ideal Patient | Wide range of anxiety, depression, and other mental health issues. | Individuals with severe emotional dysregulation, self-harm, suicidal behaviors, Borderline Personality Disorder, co-occurring substance use disorders, eating disorders, and other complex, difficult-to-treat conditions. |
The Four Core Skill Modules of DBT
DBT is a skills-based treatment that teaches practical strategies for daily life. These are the four core modules:
- Mindfulness: This skill teaches you to be present and aware without judgment. It’s crucial for noticing cravings and urges without automatically reacting, allowing you to observe thoughts and feelings as they pass.
- Distress Tolerance: Life is full of discomfort, and substance use can become an escape. These skills teach you how to get through intense emotions and crisis situations without making things worse (e.g., by using substances). You learn to accept reality and self-soothe in healthy ways.
- Emotion Regulation: This module focuses on understanding and managing emotions more effectively. For those with addiction, this means identifying emotions that trigger substance use and developing healthier ways to respond, reducing the need to self-medicate.
- Interpersonal Effectiveness: Addiction often strains relationships. These skills teach you how to ask for what you need, say no, and maintain self-respect in your relationships. This helps you build a strong, sober support network.
How DBT for Addiction Works: A Targeted Approach to Recovery
For individuals with substance use disorders (SUDs), recovery is often complicated by intense emotions and impulsive behaviors. DBT for addiction shines by addressing the underlying emotional dysregulation and skill deficits that drive substance use, not just the addiction itself.
We understand that emotions can be triggers. A wave of anxiety or a surge of anger can feel unbearable, leading to the impulse to use. DBT breaks this cycle by providing concrete strategies to manage these internal experiences without resorting to substances. It’s about learning to surf the urge rather than being drowned by it.
Adapting DBT for Substance Use Disorders (SUDs)
DBT principles are highly effective for SUDs because emotional dysregulation and impulsivity are core features of both addiction and BPD. The adapted version, DBT-SUD, introduces several key concepts:
- Dialectical Abstinence: This is a cornerstone of DBT for addiction. It balances a commitment to abstinence (change) with the acceptance that a lapse is not a total failure but a problem to be solved (acceptance). This approach reduces shame, encourages a quick analysis of what went wrong, and helps the individual get back on track swiftly.
- SUD-Specific Targets: Therapy actively targets decreasing substance abuse, alleviating withdrawal, diminishing cravings, and avoiding triggers. Behavioral chain analysis is a critical tool used to break down the sequence of events leading to substance use to identify points for intervention.
- Attachment Strategies: To combat the tendency for some to disengage from treatment, DBT-SUD uses specific strategies to keep individuals engaged, such as proactive check-ins and creating plans for re-engagement if contact is lost.
The comprehensive nature of DBT—with individual therapy, group skills training, phone coaching, and a therapist consultation team—is crucial for its success. Phone coaching, in particular, offers real-time support during a crisis, which is a significant factor in why evidence for DBT in treating addiction has grown.
The Evidence Behind DBT for Addiction
The efficacy of DBT for addiction is well-supported by research, especially for individuals with co-occurring disorders. The statistics are compelling:
- High Remission Rates: A remarkable 87.5% of those with substance dependence who received DBT achieved full remission for at least 4 weeks, compared to only 33.3% in comparison treatment groups.
- Improved Treatment Retention: DBT excels at keeping people engaged, with 64% remaining in treatment compared to just 27% in treatment as usual (TAU).
- Objective Reductions: Reductions in drug abuse were not just self-reported; they were confirmed through structured interviews and urinalyses.
- Long-Term Benefits: DBT subjects sustained improvements in social and global adjustment at a 16-month follow-up, highlighting DBT’s ability to foster lasting change.
- Effective for Complex Cases: For opiate-dependent individuals with BPD, a population often considered difficult to treat, DBT subjects were the only ones who maintained reductions in opiate abuse during the final months of one study.
These findings show that DBT equips individuals with tools for sustained recovery. For more information on treatments backed by solid research, explore our resources on evidence-based treatment.
Key Mechanisms: How DBT Skills Interrupt the Addiction Cycle
How do DBT skills interrupt the addiction cycle? By equipping individuals with the resources to manage the intense states that precede substance use.
- Emotion Regulation Skills: Many people use substances to cope with painful emotions. DBT teaches how to manage these feelings effectively. By reducing vulnerability to negative emotions, it lessens the drive to self-medicate. Research shows DBT significantly improves emotion regulation (d= –1.17).
- Distress Tolerance Skills: Life presents moments of intense discomfort that can trigger relapse. Distress tolerance skills provide concrete strategies to get through a crisis without turning to substances, such as learning to accept the moment and self-soothe in healthy ways.
- Mindfulness Skills: The ability to observe thoughts, feelings, and urges without judgment is a powerful tool. Mindfulness helps you notice early warning signs of a craving, giving you a moment to choose a skillful response rather than reacting impulsively. This reduces the tendency to avoid uncomfortable feelings (d= –0.71).
- Managing Impulsivity: Impulsivity is a hallmark of many SUDs. DBT directly addresses this by teaching skills to pause, think, and choose a different path, even when urges are strong. After DBT skills training, impulsivity levels in patients with SUDs were comparable to those of healthy controls.
The Broader Impact: DBT for Co-Occurring Disorders and Practical Considerations
The utility of DBT for addiction extends far beyond stopping substance use. It’s a holistic treatment that addresses the complex web of issues often intertwined with addiction, which is one of its greatest strengths.
What to Expect from a DBT for Addiction Program
A full, evidence-based DBT program is a commitment, but one that offers profound rewards. You can typically expect four components:
- Individual Therapy: Weekly one-on-one sessions to apply skills to your specific challenges with substance use and to help you stay motivated.
- Group Skills Training: A weekly “classroom” setting (often 2.5 hours) where you learn the four core skill modules in a supportive environment.
- Phone Coaching: In-the-moment phone support from your therapist to help you use skills during a crisis or when facing urges, preventing a situation from spiraling.
- Therapist Consultation Team: This is your therapist’s support team. They meet regularly to ensure you receive the highest quality of care according to the DBT model.
A full DBT program typically lasts around one year, providing ample time to integrate skills for lasting change. If you’re considering this path, we can help you find a DBT program near you that aligns with your needs.
Benefits for Co-occurring Behavioral Issues
DBT is effective for a wide range of co-occurring issues because it teaches fundamental emotional and behavioral skills. These behaviors often serve a similar function to substance use: attempting to regulate intense emotions or escape distress.
DBT shows promise for treating alcohol use disorder and co-occurring behavioral issues by helping individuals manage emotions more effectively. Studies show significant improvements in:
- Gambling problems
- Eating disorders (binge eating and restrictive behaviors)
- Compulsive shopping
- Compulsive sexual behavior
Challenges and Cost-Effectiveness of DBT
While DBT offers immense benefits, accessing it can present challenges, such as the need for extensive therapist training and the resources required to run a comprehensive program. However, the long-term benefits and cost-effectiveness are compelling.
Research has shown that DBT can yield significant financial savings by reducing the need for more intensive services:
- Reduced Healthcare Costs: DBT has been shown to save thousands of dollars per patient in the first year compared to treatment as usual.
- Decreased Service Use: One study found that after a year of DBT, patients had a 77% decrease in hospitalization days and an 80% decrease in emergency room contacts.
- Overall Savings: The total psychiatric service costs for patients in the same study fell dramatically in the year following treatment.
While the initial investment in DBT may seem substantial, its ability to reduce costly interventions makes it a highly cost-effective treatment in the long run.
Frequently Asked Questions about DBT for Addiction
We often hear common questions about DBT for addiction, and we’re here to provide clear answers based on our expertise and the latest research.
Is DBT only for people with Borderline Personality Disorder?
No. While originally developed for Borderline Personality Disorder (BPD), DBT is now a proven treatment for a wide range of issues where emotional dysregulation is a factor. Its skills are successfully applied to:
- Substance use disorders
- Eating disorders (binge eating and bulimia)
- Depression and anxiety disorders
- Post-traumatic stress disorder (PTSD)
- Bipolar disorder
DBT has evolved into a versatile therapy for many complex mental health and behavioral challenges.
How is ‘dialectical abstinence’ different from just being sober?
“Just being sober” is the state of not using, while “dialectical abstinence” is the skillful process used to achieve and maintain it. The key difference is how it handles setbacks.
It balances a commitment to abstinence with a non-judgmental, problem-solving approach to lapses. In traditional models, a slip can feel like a total failure, leading to shame and a full relapse. In DBT for addiction, a lapse is viewed as a learning opportunity. The focus immediately shifts to analyzing what happened and getting back on track, which reduces shame and empowers a swift recovery.
The goal is to build a “clear mind”—a state of sustained abstinence where you can skillfully manage triggers and build a life so fulfilling that the desire to escape through substances diminishes.
How long does DBT treatment for addiction usually take?
A comprehensive DBT program is an investment in lasting change and typically lasts about one year.
This duration allows sufficient time to learn, practice, and fully integrate the four skill modules into daily life. It’s not a quick fix, but a structured process designed to build a solid foundation for long-term recovery.
However, the timeframe can be flexible. Program length can be adapted based on the severity of the SUD, the presence of co-occurring conditions, and an individual’s progress and needs.
Conclusion
Navigating addiction is challenging, but DBT for addiction offers a hopeful and robust path to recovery. It goes beyond simply addressing substance use to tackle the core issues of emotional dysregulation and impulsivity. By teaching practical skills in mindfulness, distress tolerance, emotion regulation, and interpersonal effectiveness, DBT empowers you to build a life you genuinely want to live—one free from the grip of substances.
This skills-based approach is highly effective, improves treatment retention, and is remarkably cost-effective in the long run. Its ability to treat co-occurring issues makes it a truly comprehensive solution.
At Drug Rehab Headquarters, we believe in personalized, evidence-based treatment. Our certified counselors, many with lived experience, are available 24/7 to offer free, compassionate guidance. We’re here to help you or your loved one understand how DBT for addiction can fit into a holistic treatment plan and connect you with suitable options across North America. Take the first step towards a life worth living.
Get 24/7 free support from our certified counselors
