Finding Hope: Your Path to Recovery Starts Here
Suboxone treatment centers offer evidence-based medication-assisted treatment for individuals struggling with opioid addiction. Here’s what you need to know:
Quick Guide to Finding Suboxone Treatment:
- Use SAMHSA’s Practitioner Locator at samhsa.gov to find certified providers in your state
- Visit FindTreatment.gov for a comprehensive directory of treatment facilities
- Check your insurance coverage by contacting your provider directly
- Call the National Helpline at 1-800-662-4357 for 24/7 confidential support
- Look for comprehensive programs that combine medication with counseling and therapy
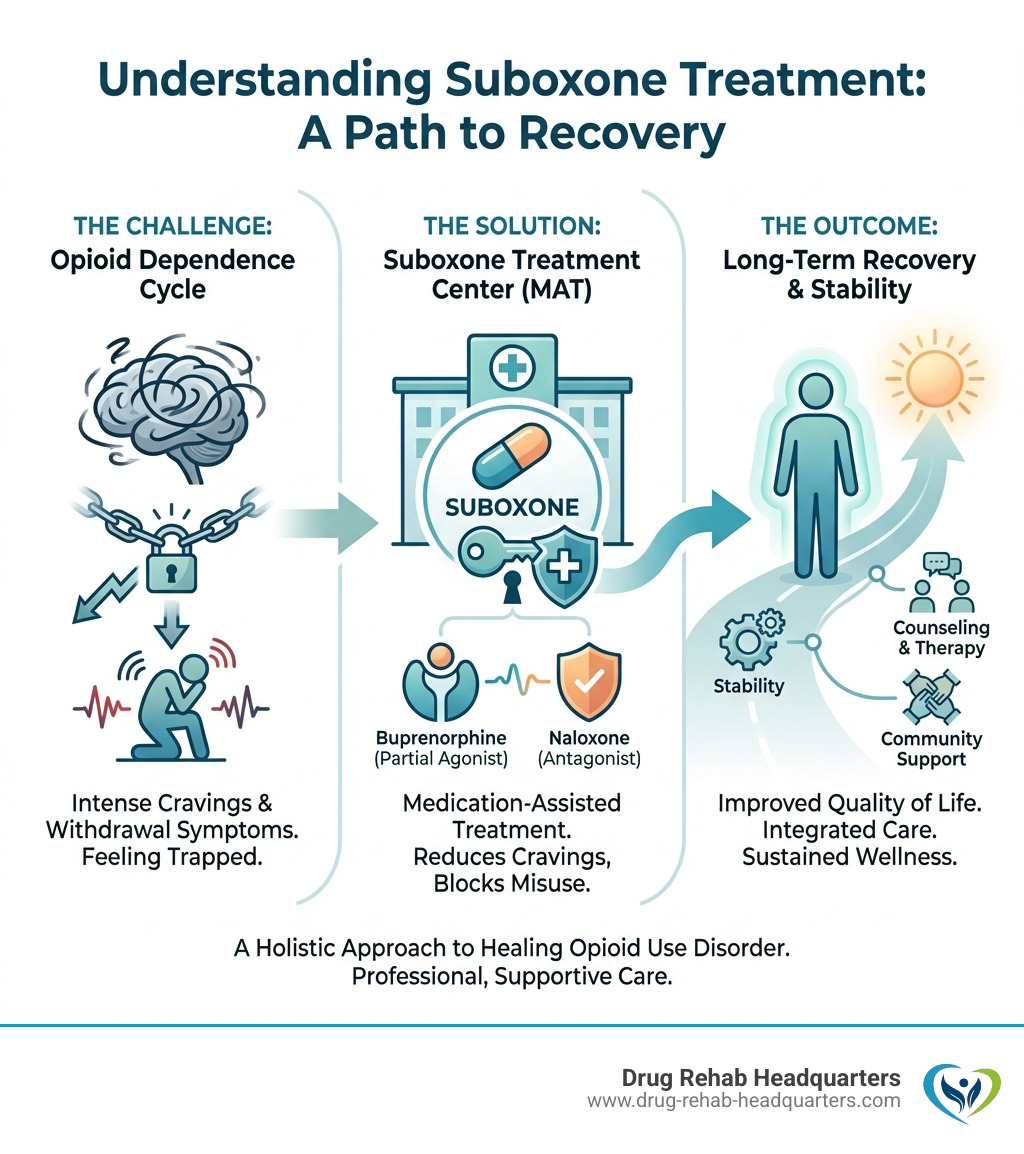
The opioid crisis impacts millions. If you’re struggling with prescription painkillers, heroin, or fentanyl, you’re not alone—and effective help is available.
Suboxone is an FDA-approved medication containing buprenorphine and naloxone. It reduces cravings and eases withdrawal symptoms, allowing you to focus on rebuilding your life. Combined with counseling, Suboxone treatment has helped countless individuals achieve lasting recovery.
This guide explains how Suboxone works, where to find care, what to expect from treatment, and how to steer insurance. Most importantly, we’ll show you that recovery is possible.
At Drug Rehab Headquarters, we connect people with reputable Suboxone treatment centers offering personalized care. Our mission is to provide accurate information and practical guidance for your recovery journey.
What Is Suboxone and How Does It Treat Opioid Addiction?
Suboxone is a crucial component of Medication-Assisted Treatment (MAT) for Opioid Use Disorder (OUD). Approved by the FDA in 2002, it’s a lifeline for many struggling with opioid addiction.
Suboxone manages the physical side of addiction by reducing cravings and easing withdrawal symptoms. This allows you to focus on the psychological work of recovery without the physical discomfort that often derails sobriety.
For more detailed information on treating opiate addiction, explore our comprehensive guide on Opiate Addiction Treatment.
The Science Behind Suboxone: Buprenorphine and Naloxone
Suboxone contains two active ingredients: buprenorphine and naloxone. This combination is designed to help you recover while deterring misuse.
Buprenorphine, a partial opioid agonist, is the primary ingredient. It attaches to the brain’s opioid receptors but only partially activates them. This is enough to stop cravings and withdrawal without causing a “high.” This “ceiling effect” means its effects don’t increase past a certain dose, lowering overdose risk compared to full opioids. It also blocks other opioids from attaching to these receptors.
Naloxone, an opioid antagonist, is the second ingredient. It deters misuse. When taken as prescribed (under the tongue), naloxone has no effect. If injected or snorted, it becomes active and triggers immediate, unpleasant withdrawal symptoms, discouraging misuse.
Suboxone and Other Buprenorphine-Based Options
Suboxone is a well-known brand, but buprenorphine is available in several formulations. Understanding the differences helps you and your provider choose the best option.
Here’s a comparison of common buprenorphine-based medications:
| Medication | Ingredients | Administration | Use Case |
|---|---|---|---|
| Suboxone | Buprenorphine + Naloxone | Sublingual film or tablet | Most common for OUD treatment, naloxone deters misuse |
| Subutex | Buprenorphine (alone) | Sublingual tablet | Used when naloxone is contraindicated (e.g., pregnancy, allergic reaction, or during induction) |
| Sublocade | Buprenorphine (alone) | Monthly extended-release injection | For moderate to severe OUD, administered by a healthcare provider after stable oral buprenorphine treatment |
| Brixadi | Buprenorphine (alone) | Weekly or monthly extended-release injection | Another injectable option for OUD, offering different dosing frequencies |
Oral forms like Suboxone and Subutex allow for flexible daily dosing, useful early in treatment. Injectables like Sublocade and Brixadi offer convenience and ensure adherence, making them great options for those stable on oral buprenorphine.
Choosing the right formulation is a personal decision made with your healthcare provider, who will consider your medical history, lifestyle, and treatment goals.
The Benefits of Suboxone in a MAT Program
Integrating Suboxone into a MAT program offers many benefits for long-term recovery, helping you rebuild a healthy life.
Some of the key benefits include:
- Reduced Cravings: Buprenorphine alleviates the intense urges that can make sobriety feel impossible, allowing you to engage in therapy.
- Eased Withdrawal Symptoms: Buprenorphine minimizes the severe physical discomfort of opioid withdrawal, making detox safer and more manageable.
- Lower Overdose Risk: By occupying opioid receptors and having a ceiling effect, buprenorphine significantly reduces the risk of overdose compared to illicit opioids.
- Improved Safety Profile: The inclusion of naloxone acts as a built-in safety mechanism, deterring misuse via injection.
- Increased Treatment Retention: When withdrawal and cravings are controlled, individuals are more likely to stay in treatment and commit to their recovery plan.
Suboxone, as part of a well-rounded MAT program, empowers you to regain control. For more insights into comprehensive recovery services, visit our Addiction Recovery Services Complete Guide.
Understanding the Risks and Side Effects of Suboxone
While a powerful tool, Suboxone is an opioid medication with its own risks, including potential physical dependence and side effects.
It’s crucial to distinguish between physical dependence and addiction. Physical dependence on Suboxone is an expected adaptation by the body. Addiction involves compulsive drug-seeking despite negative consequences. As an opioid, Suboxone maintenance leads to physical dependence.
Suboxone has a long half-life, staying in your system for a long time. Abruptly stopping it can cause prolonged, intense withdrawal symptoms, much longer than from short-acting opioids. This makes medically supervised tapering essential.
Common Side Effects and Potential Health Risks
Like any medication, Suboxone can cause side effects ranging from mild to serious. Communicate openly with your healthcare provider about any you experience.
Common side effects often include:
- Nausea and vomiting
- Drowsiness or fatigue
- Constipation
- Headache
- Sweating
- Insomnia
- Pain at the injection site (for injectable forms)
More serious, though less common, health risks can include:
- Respiratory Depression: Though less likely than with full opioids due to its ceiling effect, serious breathing problems can occur, especially when mixed with other depressants like benzodiazepines or alcohol. This can be life-threatening.
- Liver Problems: Rarely, Suboxone can cause liver damage. Signs include jaundice, dark urine, or stomach pain. Your doctor will monitor your liver function.
- Allergic Reactions: Severe allergic reactions (rash, hives, swelling, difficulty breathing) are rare but possible.
- Adrenal Insufficiency: Long-term opioid use, including buprenorphine, can lead to adrenal gland problems.
- Opioid Withdrawal Symptoms: Misuse (e.g., injection) can trigger acute withdrawal due to the naloxone.
If you experience concerning side effects like difficulty breathing, severe drowsiness, or signs of liver problems, seek immediate medical attention. We encourage you to report any negative side effects of drugs to the FDA via Information on reporting side effects to the FDA.
Signs of Suboxone Misuse or Dependence
Though designed to prevent misuse, a problematic relationship with Suboxone is possible, especially if not taken as prescribed. Recognizing the signs of misuse is crucial for getting back on track.
Signs of Suboxone misuse or dependence may include:
- “Doctor shopping” for multiple prescriptions
- Taking more than prescribed
- Combining with other substances like alcohol or benzodiazepines
- Intense cravings for Suboxone
- Withdrawal symptoms when trying to stop or reduce the dose
- Behavioral changes like apathy, slurred speech, or mood swings
- Neglecting responsibilities in favor of obtaining or using Suboxone
If you or a loved one show these signs, seek professional help. Addressing Suboxone dependence requires a medically supervised taper and comprehensive therapy. For more information, see our guide on Detox from Prescription Drugs.
How to Find and Access Suboxone Treatment Centers
Finding the right Suboxone treatment center can feel daunting, but the right resources make it manageable. We are here to simplify the process, from locating a provider to understanding your insurance.

Using Online Resources to Locate Suboxone Treatment Centers
Several excellent online resources can help you locate Suboxone treatment centers and qualified practitioners. These tools are often your first step in finding care.
- SAMHSA’s Buprenorphine Practitioner Locator: This tool from the Substance Abuse and Mental Health Services Administration (SAMHSA) helps you find practitioners authorized to treat opioid dependency with buprenorphine. This list only contains practitioners who consent to be listed and, due to recent legislative changes, may not be fully comprehensive. You can access this tool here: Buprenorphine Practitioner Locator.
- FindTreatment.gov: This is a confidential and anonymous resource for individuals seeking treatment for mental and substance use disorders in the United States.
- Opioid Treatment Program Directory: Also from SAMHSA, this directory helps you find programs that provide medication-assisted treatment for opioid addiction.
When using these locators, remember they are excellent starting points, but their information may not be exhaustive.
New Laws Expanding Access to Buprenorphine
Access to buprenorphine has significantly improved thanks to recent legislative changes. The Consolidated Appropriations Act of 2023 eliminated the federal requirement for practitioners to obtain a special waiver (the “X-waiver”) to prescribe buprenorphine for opioid use disorder.
This means that as of 2023, any practitioner with a standard DEA registration can prescribe buprenorphine for OUD. This change dramatically expands the pool of healthcare providers who can offer treatment, removing a significant barrier to care and making it easier to find a qualified doctor in your community.
Paying for Treatment and Verifying Insurance
The cost of treatment can be a concern, but options are available. Many Suboxone treatment centers accept insurance, and there are resources for those without coverage.
Here’s how to approach paying for treatment:
- Contact Your Insurance Provider: Call your insurance company to ask about your benefits for substance use disorder treatment, specifically MAT. Inquire about deductibles, co-pays, and pre-authorization requirements.
- In-Network vs. Out-of-Network: Check if the centers you are considering are in-network with your plan to lower out-of-pocket costs.
- Medicaid and Medicare Coverage: Many state Medicaid programs and Medicare cover MAT services, including Suboxone.
- Self-Pay Options: If you don’t have insurance, many centers offer self-pay options or sliding scale fees based on income. Always inquire about financial assistance.
At Drug Rehab Headquarters, we can help you verify your insurance coverage. For more information, visit our page on Addiction Treatment.
Specialized Treatment for Specific Populations
Everyone’s journey is unique, and some individuals benefit from specialized programs. Many Suboxone treatment centers offer targeted support for various populations.
Examples of specialized programs include:
- Programs for Veterans: Services designed to address the unique challenges faced by veterans, including co-occurring PTSD.
- First Responders: Programs that understand the high-stress environments that can contribute to addiction for firefighters, police, and others.
- Pregnant Women: A specialized approach to ensure the health of both mother and baby. Subutex (buprenorphine alone) is often preferred.
- Young Adults: Programs that cater to the developmental stage, social needs, and educational goals of young adults.
These approaches ensure treatment addresses the addiction and its underlying factors. For a complete guide, explore our Addiction Treatment Center Complete Guide.
What to Expect from a Suboxone Treatment Program
A Suboxone treatment program is a comprehensive approach to recovery. It’s not just about medication; it’s about healing your whole self. Quality Suboxone treatment centers provide individualized care that integrates medication with therapy for your physical and mental well-being. The focus is on a personalized plan, as there’s no one-size-fits-all solution. This holistic approach, including dual diagnosis treatment for co-occurring mental health conditions, sets the stage for lasting recovery.
Comprehensive Services Offered at Suboxone Treatment Centers
A reputable Suboxone treatment center offers a full spectrum of care to support every stage of recovery. Typically, you can expect:
- Medical Evaluation and Induction: A thorough assessment to see if Suboxone is right for you, followed by a managed induction phase to stabilize your dose.
- Custom Treatment Plans: A plan custom to your specific needs, goals, and circumstances.
- Medication Management: Regular check-ups to monitor your dosage, manage side effects, and ensure the medication is effective.
- Counseling and Therapy: Individual and group therapy to address the root causes of addiction and develop coping skills.
- Case Management: Help coordinating care and connecting you with community resources (housing, employment, etc.).
- Aftercare Planning: A robust plan for lifelong recovery, including ongoing therapy or support groups.
For a deeper dive, refer to our Addiction Treatment Center Complete Guide.
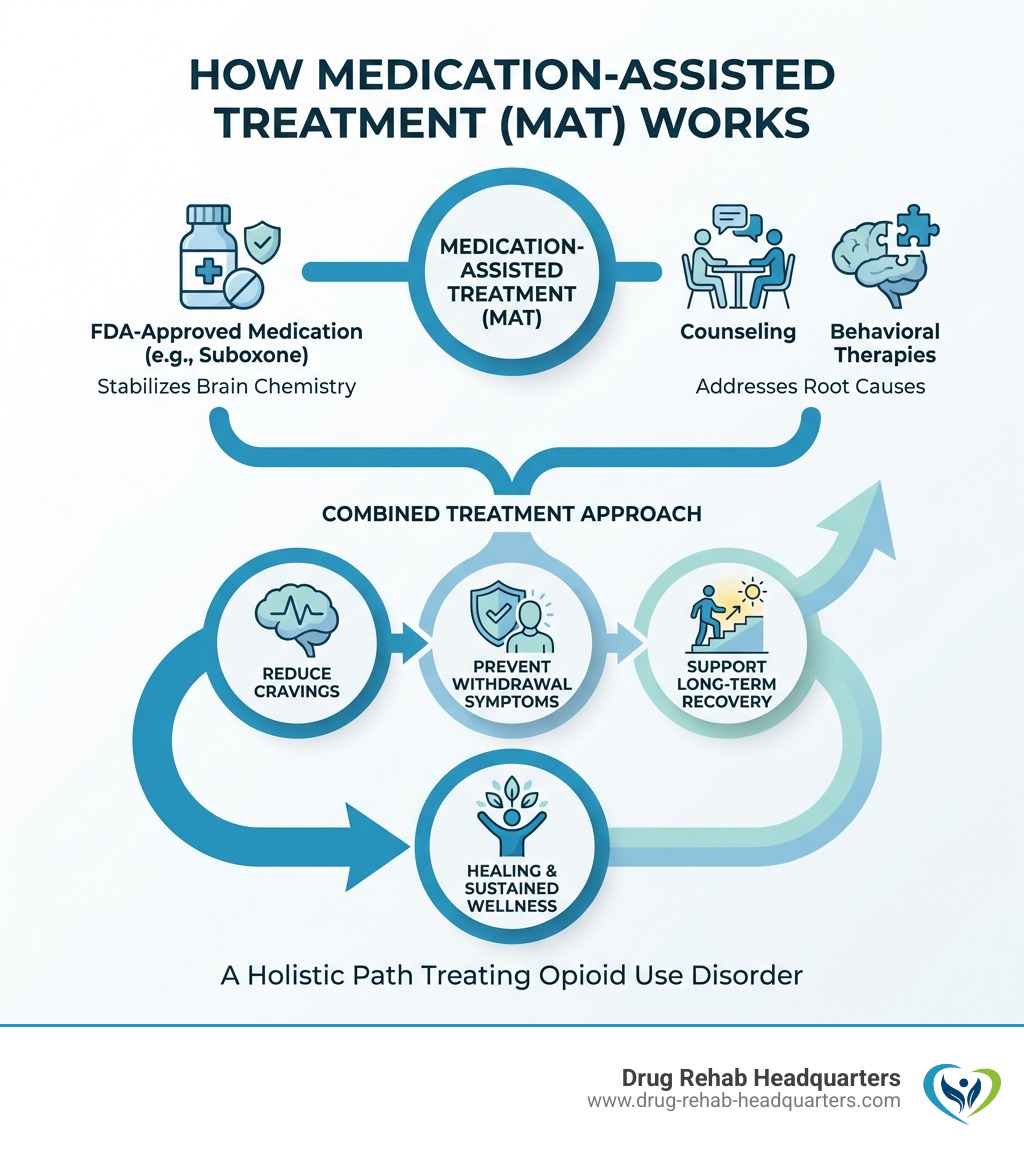
The Crucial Role of Behavioral Therapy and Counseling
MAT with Suboxone is most effective when combined with behavioral therapy. Suboxone provides the stability needed to engage in the therapeutic work that addresses the psychological side of addiction.
Common therapeutic approaches include:
- Cognitive Behavioral Therapy (CBT): Helps you identify and change negative thought patterns and behaviors related to substance use, teaching healthier coping skills.
- Dialectical Behavior Therapy (DBT): Often used for co-occurring conditions, DBT teaches skills in mindfulness, distress tolerance, emotion regulation, and interpersonal effectiveness.
- Group Therapy: Fosters a sense of community and reduces isolation by sharing experiences with peers.
- Family Counseling: Helps improve communication, rebuild trust, and heal relationships damaged by substance use.
These therapies help you build a strong foundation for a life in recovery.
Levels of Care: From Detox to Outpatient Support
Suboxone treatment centers offer a continuum of care with different levels of support. Your journey may start with intensive care and transition to less restrictive settings as you gain stability.
- Medical Detox: The first step for many, providing safe, supervised management of withdrawal symptoms. Suboxone induction often begins here.
- Inpatient/Residential Treatment: 24/7 support in a structured, trigger-free environment with intensive therapy.
- Partial Hospitalization Programs (PHP): Also called “day treatment,” this provides intensive clinical care during the day while you return home or to sober living at night.
- Intensive Outpatient Programs (IOP): Structured therapy for several hours a day, a few days a week, allowing you to maintain daily responsibilities.
- Standard Outpatient: The least restrictive level, involving weekly therapy sessions for those transitioning to independent living.
For a comprehensive understanding of detox, please refer to our Detox Treatment guide.
Addressing Co-Occurring Mental Health Conditions
It’s common for opioid use disorder to co-occur with mental health conditions like depression, anxiety, or PTSD. This is a “dual diagnosis,” and treating both simultaneously is vital for recovery.
Reputable Suboxone treatment centers offer integrated treatment, addressing mental health as part of your overall recovery plan. This may include:
- Integrated Therapy: Sessions with therapists who specialize in both addiction and mental health.
- Medication Management for Mental Health: A psychiatrist can manage medications for mental health conditions alongside Suboxone.
- Holistic Care: Approaches like mindfulness, yoga, or art therapy to promote overall well-being.
Treating co-occurring conditions helps resolve underlying issues, paving the way for a more stable recovery.
Frequently Asked Questions about Suboxone Treatment
We know you might have many questions about Suboxone treatment centers and the recovery process. Here are answers to some of the most common inquiries we receive.
How long does Suboxone treatment last?
The duration of Suboxone treatment varies significantly from person to person. There’s no set timeline, as recovery is a highly individualized journey. Some individuals may stay on Suboxone for a few months, while others may benefit from maintenance treatment for several years or even indefinitely.
The goal is always to achieve stability and improve your overall quality of life. Your doctor will work with you to determine the appropriate duration, considering your progress, stability, and personal goals. When the time is right, a medically supervised tapering plan will be implemented to slowly reduce your dosage, minimizing withdrawal symptoms. Collaboration with your doctor is key throughout this process.
Can you become addicted to Suboxone?
This is a critical question. As we discussed earlier, physical dependence on Suboxone is expected because it’s an opioid medication. Your body will adapt to its presence. However, physical dependence is different from addiction.
Addiction to Suboxone, or misuse, occurs when an individual compulsively seeks and uses the medication despite negative consequences, often deviating from their prescribed dosage or method of administration. While Suboxone contains naloxone to deter misuse, it is still possible. The risk of developing an addiction to Suboxone is significantly lower than with full opioid agonists, especially when taken as prescribed and under medical supervision within a comprehensive treatment program. The crucial aspect is the professional oversight and the integration of therapy, which helps address the psychological drivers of addiction.
Is Suboxone treatment effective for long-term recovery?
Yes, Suboxone treatment, as part of a comprehensive MAT program, is highly effective for long-term recovery from opioid use disorder. Research consistently shows that individuals who combine Suboxone with behavioral therapy and counseling have significantly better outcomes than those who attempt recovery without medication.
The benefits include:
- High Success Rates: When combined with therapy, Suboxone significantly increases the likelihood of sustained sobriety.
- Reduces Illicit Opioid Use: By managing cravings and withdrawal, Suboxone helps individuals stop using illicit opioids.
- Lowers Overdose Mortality: Studies have shown that MAT, including buprenorphine, dramatically reduces the risk of fatal opioid overdose.
- Improves Overall Functioning: Individuals in MAT programs often experience improvements in their health, relationships, employment, and overall quality of life.
Suboxone is a powerful tool for recovery, not a “cure.” It provides the stability needed to engage in the hard work of therapy and lifestyle changes, empowering you to build a fulfilling life free from opioid addiction.
Take the First Step Toward Recovery Today
We hope this guide has shed some light on Suboxone treatment centers and the path to recovery from opioid use disorder. Suboxone, when used as part of a comprehensive medication-assisted treatment program, is an incredibly effective tool that can help you reclaim your life. Comprehensive treatment that combines medication with behavioral therapy and counseling is the most successful approach.
Recovery is not just a possibility; it’s a reality that countless individuals have achieved. We believe in your strength and your ability to heal.
At Drug Rehab Headquarters, we are here to support you every step of the way. Our 24/7 free support from certified counselors, many with lived experience, means you’ll receive personalized guidance to find suitable, evidence-based, holistic treatment options. We can connect you with the right Suboxone treatment centers across Alabama, Alaska, Arizona, Arkansas, California, Colorado, Connecticut, Delaware, Florida, Georgia, Hawaii, Idaho, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Montana, Nebraska, Nevada, New Hampshire, New Jersey, New Mexico, New York, North Carolina, North Dakota, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, South Carolina, South Dakota, Tennessee, Texas, Utah, Vermont, Virginia, Washington, West Virginia, Wisconsin, and Wyoming.
Don’t let another day pass in the shadow of addiction. Reach out today, and let us help you find the hope and healing you deserve.

