
Why a Relapse Prevention Program is Essential for Long-Term Recovery
A relapse prevention program is a structured, skills-based approach designed to help individuals in recovery identify high-risk situations, develop effective coping strategies, and maintain sobriety by understanding that relapse is a process with distinct stages—not a single event or personal failure.
Key Components of an Effective Relapse Prevention Program:
- Identifying Personal Triggers – Recognize emotional states, people, places, and situations that increase risk
- Developing Coping Skills – Build behavioral and cognitive strategies to manage cravings and stress
- Creating a Written Action Plan – Document warning signs, emergency contacts, and specific responses to high-risk scenarios
- Building Support Networks – Engage with sponsors, therapists, peer groups, and family members
- Ongoing Monitoring – Track emotional and mental states before physical relapse occurs
Addiction is a chronic disease, and research shows that 40% to 60% of people with substance use disorders experience relapse after treatment. This statistic highlights why a proactive plan is critical. Recovery is a journey, and relapse prevention is about preparing with the awareness and tools to recognize warning signs early, when intervention is most effective.
Understanding that relapse happens in stages—emotional, mental, and physical—gives you the power to intervene early. A relapse prevention program transforms this process into concrete, actionable steps.
At Drug Rehab Headquarters, we’ve helped countless individuals and families steer the complexities of addiction recovery by providing expert guidance on evidence-based relapse prevention programs that work. Our mission is to connect you with the resources, information, and support systems that give you the best chance at building a relapse-proof life beyond initial treatment.
Understanding Relapse: A Process, Not a Failure
When we talk about relapse in addiction recovery, it’s easy to view it as a sudden failure. However, relapse is not an event that happens out of the blue; it’s a gradual process of shifts in feelings, thoughts, and behaviors. Understanding this distinction is crucial, as it empowers us to intervene long before a physical relapse occurs.
Think of recovery as a long, winding path. A setback doesn’t mean the journey is over; it’s a rough patch that requires a different approach or a renewed commitment to recovery tools.
Normalizing relapse means acknowledging its prevalence—studies show relapse rates for substance use disorders are comparable to other chronic diseases like asthma. However, normalizing it does not mean minimizing its urgency. Instead, we can approach it as a learning opportunity to identify what went wrong and refine our strategies for sustained sobriety.
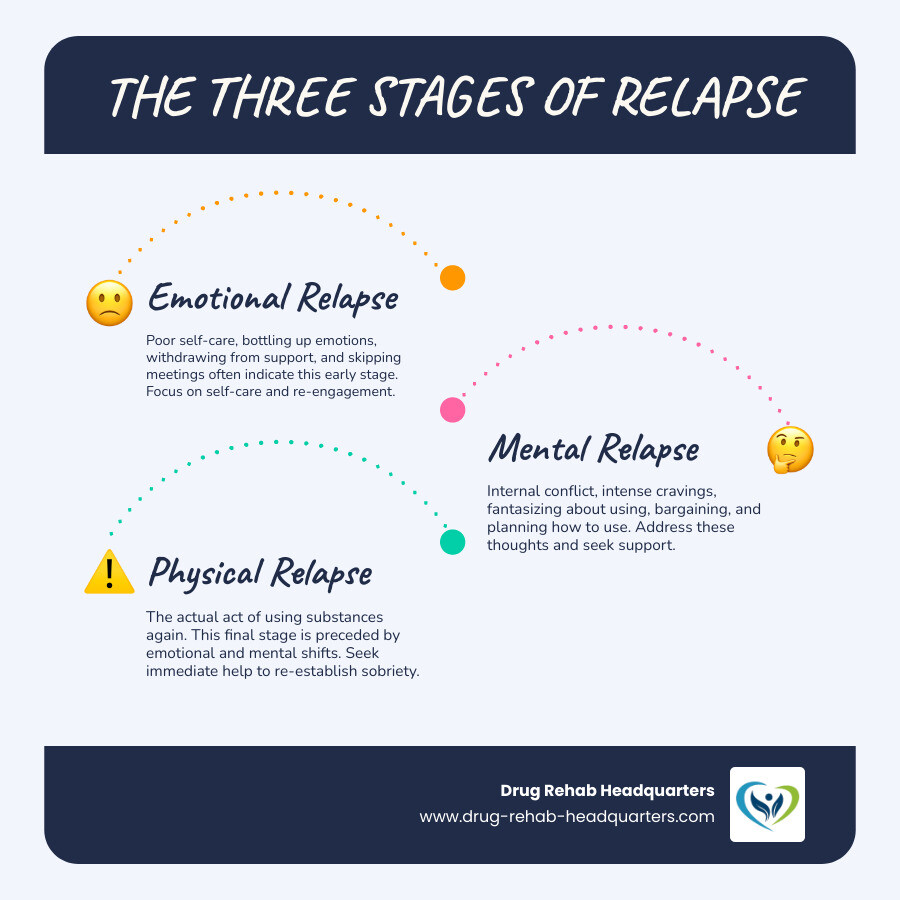
The Three Stages of Relapse
As highlighted in the infographic above, relapse unfolds in distinct stages, offering multiple opportunities for intervention. Recognizing these stages early can make all the difference:
-
Emotional Relapse: In this earliest stage, you aren’t thinking about using, but your emotions and behaviors are setting the stage for it. Signs include bottling up emotions, isolation, mood swings, poor self-care (eating, sleeping), and skipping support meetings. It’s a period of emotional vulnerability and declining coping skills.
-
Mental Relapse: Here, thoughts of using begin to surface. An internal conflict arises, featuring cravings, fantasizing about past use, and bargaining with yourself (“just one time”). You might glamorize past use or try to justify it. This is the internal battle between staying sober and giving in.
-
Physical Relapse: This final stage is the act of consuming a substance after a period of abstinence. While a serious setback, it doesn’t mean all progress is lost. The goal is to recognize it quickly, minimize its duration, and re-engage with your relapse prevention program. Understanding the impacts of substance use, including dangerous withdrawal symptoms, is critical. Learn more in our Drug Withdrawal Symptoms Complete Guide.
Lapse vs. Relapse: What’s the Difference?
The terms “lapse” and “relapse” are often used interchangeably, but their distinction is crucial. Understanding the difference can prevent a minor slip-up from becoming a full return to substance use.
A lapse is a “slip-up” or a single, brief instance of substance use, after which the person quickly regains control and recommits to recovery.
A relapse implies a more sustained return to uncontrolled substance use, signifying a loss of control and a need to re-engage with treatment.
The Abstinence Violation Effect (AVE) is when a lapse is viewed as a complete failure, leading to guilt, shame, and hopelessness. This negative spiral can lead to continued use. The goal is to reframe a lapse as a learning experience, not a failure.
Here’s a table comparing the characteristics and recommended responses for a lapse versus a relapse:
| Feature | Lapse | Relapse |
|---|---|---|
| Definition | A single, brief instance of substance use. | A sustained return to previous patterns of substance use; loss of control. |
| Mindset | “I made a mistake, but I can get back on track.” | “I’ve failed completely, so I might as well keep using.” (Abstinence Violation Effect often present) |
| Duration | Short-lived; quickly followed by renewed commitment to abstinence. | Prolonged; often leads to a return to problematic use over days, weeks, or longer. |
| Emotional State | Guilt, disappointment, but motivation to correct course remains. | Overwhelming shame, hopelessness, despair, leading to continued use to cope. |
| Handling | Reframing as a learning experience: Analyze what led to it, what coping skills were missing, and what can be done differently next time. Immediately recommit to your relapse prevention program. | Re-evaluation and re-engagement: Seek professional help, re-enter treatment if necessary, review and adjust the entire relapse prevention program. |
When a lapse occurs, the most important thing is how we respond. Instead of succumbing to the AVE, we encourage individuals to view it as a valuable piece of data. What triggered it? What thoughts led up to it? By exploring these questions, we turn a potential downfall into a stepping stone for stronger, more resilient recovery.
Identifying Your Personal Risk Factors and Triggers
Self-awareness is the cornerstone of any effective relapse prevention program. We must become detectives of our own lives, identifying the specific internal (thoughts, feelings) and external (people, places, situations) risk factors and triggers that could jeopardize sobriety.
For many, substance use became a way to cope with underlying mental health issues. Addressing these co-occurring disorders is vital for long-term recovery. Our guide on Dual Diagnosis Treatment Facility provides more insights into integrated care. Understanding what makes us vulnerable is the first step toward building robust defenses.
Common Triggers and High-Risk Situations
Triggers are cues that provoke cravings. High-risk situations are contexts where we are more susceptible to these triggers. Let’s break down some of the most common ones:
-
HALT (Hungry, Angry, Lonely, Tired): This acronym highlights fundamental states that increase vulnerability. When hungry, angry, lonely, or tired, judgment is impaired and resilience is low, making old habits tempting. Prioritizing self-care to avoid these states is a crucial part of a relapse prevention program.
-
Negative Emotional States: Feelings like sadness, anxiety, stress, and boredom are common triggers. Without healthy coping mechanisms for these emotions, the instinct can be to turn to substances for temporary relief.
-
Interpersonal Conflict: Arguments or strained relationships with loved ones create stress. The emotional turmoil can trigger a desire to escape through substance use.
-
Social Pressure: Being around people who are actively using or in environments where use is normalized can create immense pressure to conform, especially in early recovery.
-
Positive Emotional States: Even positive emotions like excitement or celebration can be triggers. If substance use was tied to happy events, it can be hard to experience joy without that association. Thinking “I can handle just one” during a celebration is a classic high-risk scenario.
-
Environmental Cues (People, Places, and Things): These are external reminders of past use, such as driving past an old bar or seeing specific people. These cues can evoke powerful cravings due to classical conditioning.
The Impact of Co-Occurring Issues and Lifestyle
Broader life factors and mental health conditions significantly influence relapse risk:
-
Stress Management: Unmanaged chronic stress is a leading contributor to relapse. Developing healthy ways to manage stress, such as exercise, mindfulness, or hobbies, is paramount.
-
Untreated Mental Health Issues: Many individuals with substance use disorders also struggle with co-occurring conditions like depression, anxiety, or PTSD. If left untreated, symptoms can lead to self-medication. This is why integrated treatment for dual diagnosis is so important. For those struggling with anxiety, find appropriate care with Anxiety Disorder Treatment Centers.
-
Lifestyle Imbalance: A life that lacks balance—too much work, not enough rest, poor nutrition—depletes our reserves and makes us more susceptible to urges.
-
Lack of Routine: Predictable routines offer structure and a sense of normalcy, which are incredibly grounding in recovery. A lack of routine can lead to boredom and increased risk.
-
Unrealistic Expectations: Expecting immediate happiness or a problem-free life after treatment leads to disappointment. When these unrealistic expectations aren’t met, it can cause discouragement and vulnerability to relapse. Recovery is a gradual process of growth with occasional setbacks.
Designing Your Personal Relapse Prevention Program
A relapse prevention program is a personal blueprint for maintaining sobriety. Its beauty lies in its proactive nature: we don’t wait for a crisis; we prepare for it. This involves creating a written plan customized to our unique triggers and strengths.

Creating a detailed, written plan provides a clear roadmap for navigating challenges. As researchers Marlatt and Gordon, pioneers in the field, emphasized, Relapse Prevention (RP) is a structured, evidence-based approach that helps individuals identify high-risk situations and develop coping strategies. This approach has strong empirical support. You can learn more about its strategies and theoretical support here: Relapse Prevention: Early warning signs and important coping skills.
Key Components of a Successful Relapse Prevention Program
A robust relapse prevention program incorporates several essential elements to create a comprehensive safety net:
- Identifying Warning Signs: List the specific feelings, thoughts, and behaviors that typically precede your substance use. These are your personal red flags.
- Developing Healthy Coping Skills: For each trigger, brainstorm and practice alternative, healthy coping mechanisms like exercise, meditation, journaling, or talking to a friend.
- Creating an Emergency Contact List: Have a readily accessible list of people to call when tempted to use, including your sponsor, therapist, or supportive family members.
- Planning for Cravings: Cravings are normal. Develop a plan to manage them, such as distraction techniques, “urge surfing,” or reminding yourself they are temporary.
- Establishing Healthy Routines: Structure provides stability. This includes consistent sleep, regular meals, exercise, and dedicated time for self-care and recovery activities. Continuing care services, like those in our Post Rehab Drug Rehab Aftercare guide, are crucial for maintaining these routines.
Integrating Evidence-Based Techniques
Modern relapse prevention programs often integrate a variety of proven therapeutic techniques.
-
Cognitive-Behavioral Therapy (CBT): A cornerstone of relapse prevention, CBT helps you identify and change problematic thinking patterns and behaviors. You learn to challenge automatic thoughts (like “just one won’t hurt”) and develop healthier responses. A key component, cognitive restructuring, helps reframe a lapse as a learning opportunity, preventing the Abstinence Violation Effect.
-
Mindfulness-Based Relapse Prevention (MBRP): MBRP combines mindfulness with relapse prevention. It teaches you to observe thoughts, feelings, and cravings without judgment. This practice, known as urge surfing, helps you see cravings as temporary waves, not commands. It creates space between a trigger and your reaction, allowing you to choose a healthier response. Explore this with a 3 Minute Body Scan Meditation video.
-
Motivational Interviewing (MI): MI is a collaborative approach that helps resolve ambivalence about changing behavior. It strengthens your motivation and commitment to your relapse prevention program, especially during challenges. Studies show its effectiveness in addiction treatment.
-
Contingency Management (CM): CM uses motivational incentives, like vouchers or small rewards, to reinforce positive behaviors like abstinence. These programs are highly effective, providing tangible encouragement during crucial recovery stages.
The Power of Connection: Support Systems in Recovery
Recovery is not a solitary endeavor; isolation is a dangerous trap. Building a strong, sober support network is vital for long-term success. Connection provides strength, accountability, and belonging to combat the loneliness of addiction. This network of professionals, loved ones, and peers reinforces your relapse prevention program and helps you steer sober living.
The Role of Professional Help in a Relapse Prevention Program
Engaging with mental health professionals is a cornerstone of an effective relapse prevention program. Their expertise provides custom strategies and unbiased support.
-
Benefits of Professional Guidance: Therapists and counselors specializing in addiction can help you dig deeper into the root causes of substance use, develop advanced coping skills, and address co-occurring mental health issues.
-
Medication-Assisted Treatment (MAT): MAT can be a powerful tool in preventing relapse.
- Naltrexone reduces relapse risk for alcohol use disorder by blocking the euphoric effects of alcohol and opioids.
- Acamprosate helps reduce alcohol cravings.
- For opioid dependence, methadone and buprenorphine are critical for reducing cravings and withdrawal.
Combined with therapy, these medications significantly improve outcomes. For more information, see our Addiction Treatment Center Complete Guide.
-
Interprofessional Healthcare Teams: Effective relapse prevention often involves a team approach. Primary care clinicians, nurses, and pharmacists can collaborate to ensure all aspects of your health are addressed.
Peer Support Groups and Sponsorship
Peer support is invaluable, offering empathy, shared experience, and practical advice.
-
12-Step Programs: Organizations like Alcoholics Anonymous (AA) and Narcotics Anonymous (NA) provide structured pathways to recovery through mutual support. Regular meetings and working the steps with a sponsor offer consistent reinforcement.
-
Non-12-Step Alternatives: For those who prefer different approaches, groups like SMART Recovery offer science-based, self-empowering programs focused on self-management and cognitive-behavioral techniques.
-
The Role of a Sponsor or Mentor: A sponsor, typically someone with sustained recovery, provides one-on-one guidance, support, and accountability. Peer recovery coaches also offer personalized support and mentorship.
Frequently Asked Questions about Relapse Prevention
We understand that recovery brings many questions, especially concerning potential setbacks. Here, we address some of the most common inquiries about relapse prevention programs.
What are the first signs of a relapse?
The earliest signs are almost always emotional and behavioral, long before any substance use. This “emotional relapse” stage includes:
- Mood swings and irritability
- Isolating yourself from friends, family, and support groups
- Poor self-care, such as neglecting hygiene, healthy eating, or sleep
- Bottling up emotions, leading to pent-up stress
- Skipping support meetings or therapy sessions
- Developing negative thought patterns
Recognizing these signs in yourself or a loved one is crucial for early intervention.
How do you create a relapse prevention plan?
Creating a personalized relapse prevention program is a proactive process. A good plan is written down and includes:
- Identify Your Personal Triggers: List the specific situations, people, places, and emotions that led to past use.
- Develop Coping Strategies: For each trigger, list a healthy, alternative way to cope, such as exercise, mindfulness, or calling a friend.
- Create an Emergency Contact List: Have a list of supportive people (sponsor, therapist, family) to call when you feel an urge.
- Plan for Cravings: Detail specific actions to take when a craving hits, like distraction techniques or urge surfing.
- Establish a Healthy Routine: Outline a daily schedule with consistent meals, exercise, sleep, and recovery activities.
- Review and Update: Keep the plan accessible and review it regularly, updating it as you grow in your recovery.
Can you recover from a relapse?
Absolutely, unequivocally YES. A relapse is not a failure; it is a setback and an opportunity for profound learning. The chronic nature of addiction means setbacks can occur, but they do not negate your progress or end your recovery journey.
When a relapse happens, it provides invaluable information about your relapse prevention program. It helps you:
- Reassess and Refine: Analyze what led to the relapse to adjust your plan and make it more robust.
- Strengthen Coping Skills: A relapse highlights where new or stronger coping mechanisms are needed.
- Recommit with More Knowledge: Use the experience to fuel a stronger recommitment to sobriety.
- Seek Additional Support: A relapse is often a signal to intensify professional help or re-engage with your support network.
We emphasize that recovery is a process of continuous learning. If you or a loved one experiences a relapse, reach out immediately. Our certified counselors are here to provide compassionate guidance and connect you with the resources needed to get back on track stronger than before.
Take the Next Step in Your Recovery Journey
We’ve explored the critical role of a relapse prevention program in sustaining long-term sobriety. We’ve seen that relapse is a process with distinct stages, not a sudden failure, and that understanding the difference between a lapse and a full relapse can empower us to steer setbacks effectively. From identifying personal triggers like the HALT states, to integrating evidence-based techniques like CBT and MBRP, to building robust support systems, every element plays a vital role in building a relapse-proof life.
Your journey to recovery is unique, and while challenges may arise, you don’t have to face them alone. Empowering yourself with a personalized relapse prevention program is not just about avoiding old habits; it’s about building a fulfilling, balanced life that makes sobriety the most appealing choice every day.
At Drug Rehab Headquarters, we are dedicated to connecting individuals across North America, including states like Alabama, Alaska, Arizona, Arkansas, California, and many more, to the best addiction treatment and relapse prevention programs available. Our certified counselors, many with lived experience, are available 24/7 to offer free, personalized guidance, helping you find suitable, evidence-based, holistic treatment options.
Don’t let the fear of relapse overshadow the hope of lasting recovery. Take the proactive step today to strengthen your journey.

